Wearable devices are transforming occupational therapy, allowing therapists to monitor patients beyond clinic visits. This approach provides precise data on movement, therapy adherence, and progress, enabling tailored treatment adjustments. Remote Therapeutic Monitoring (RTM) uses devices like motion trackers and smartwatches to track metrics such as range of motion, pain levels, and exercise compliance. Medicare supports RTM with reimbursement codes, making it a recognized therapy service.
Key benefits include:
- Improved adherence: Patients using RTM complete 3.3x more exercises.
- Better outcomes: Over 30% improvements in pain and function.
- Custom alerts: Triggers for missed sessions, pain spikes, or overactivity.
- Data-driven care: Therapists refine plans based on trends.
RTM tools like the AIH Health App integrate with wearable devices to provide real-time feedback while ensuring compliance with billing and privacy standards. By combining wearable technology, data analysis, and personalized protocols, RTM is reshaping how therapy is delivered and managed.
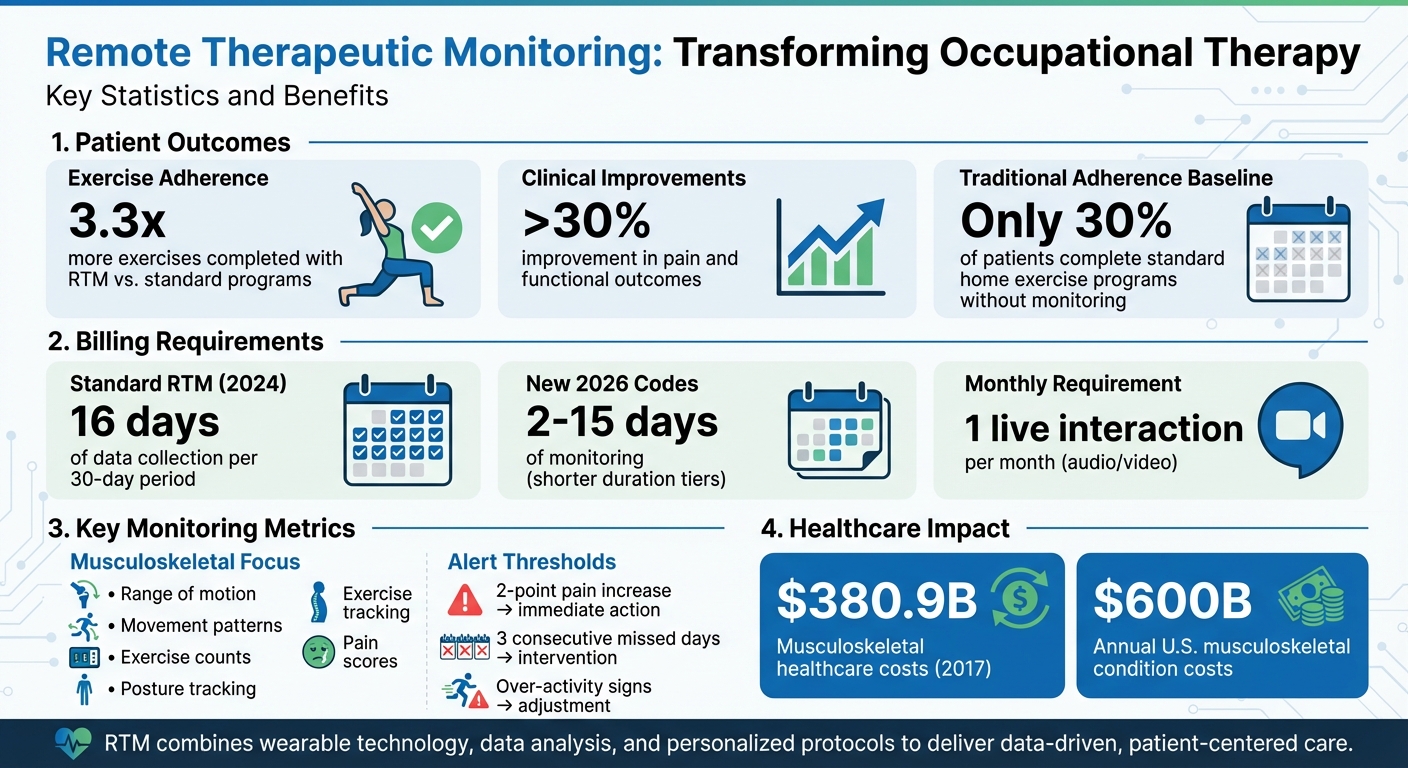
Remote Therapeutic Monitoring Benefits and Key Metrics for Occupational Therapy
Wearable Technologies Enabling Remote Therapeutic Monitoring for Post-Stroke Rehabilitation
sbb-itb-44aa802
Core Elements of Effective RTM Protocols
Creating effective Remote Therapeutic Monitoring (RTM) protocols hinges on a clear strategy: identifying what to monitor, when to intervene, and how data will be shared. Without these foundational elements, the collected data risks becoming disconnected and fails to drive meaningful clinical decisions.
Data Collection Parameters
RTM protocols typically focus on key metrics related to musculoskeletal and respiratory conditions. For example, musculoskeletal disorders alone accounted for an enormous $380.9 billion in healthcare costs in 2017, emphasizing the need for precise tracking.
Essential metrics for musculoskeletal RTM include range of motion, movement patterns, exercise counts, and posture [17,18]. These metrics provide the data needed to refine occupational therapy plans. Equally important are subjective inputs such as pain scores, symptom logs, exercise difficulty ratings, and functional status assessments, which offer a more complete view of the patient’s progress [15,16]. For respiratory-focused protocols, tracking parameters like inhaler usage frequency, spikes in rescue inhaler use, and environmental triggers is critical. When cognitive-behavioral therapy is part of the treatment plan, additional inputs such as homework completion rates, mood scoring, and sleep logs should be included.
"RTM focuses on musculoskeletal and respiratory systems, therapy adherence, and therapy response." – Vianova
To meet standard RTM billing requirements, a minimum of 16 days of data collection within a 30-day period is necessary for device supply reimbursement. However, new 2026 coding updates introduce shorter duration tiers, covering 2–15 days of monitoring. This flexibility allows protocols to be tailored to the therapy episode rather than rigid billing cycles [16,18].
Alert Thresholds and Notifications
Defining alert thresholds is essential for bridging clinical expertise with technology. For example, set triggers for immediate action, such as a 2-point increase in pain scores, three consecutive days of missed exercises, or signs of over-activity that could lead to re-injury [18,20].
Real-time dashboards are a game-changer, giving therapists instant access to patient progress between visits. This is crucial because only about 30% of patients complete standard home exercise programs without monitoring, whereas RTM users complete 3.3 times more sessions. This increased engagement has been linked to over 30% improvements in pain and functional outcomes compared to traditional methods.
Protocols should also differentiate between under-performance due to pain and recovery plateaus, as each requires a unique clinical approach [20,21]. Mid-cycle checkpoints can help identify patients who are not meeting the required data-day threshold, ensuring both compliance with therapy and billing eligibility. Additionally, protocols must include at least one real-time interaction per month (via audio or video) to meet clinical management standards – automated texts alone are insufficient [18,20]. These structured alerts and interactions ensure smooth integration into digital workflows.
Integration with Digital Health Platforms
Selecting the right technology platform is critical for RTM success. The platform must qualify as Software as a Medical Device (SaMD) under FDA guidelines; general wellness apps or SMS reminders won’t meet RTM billing standards [16,18]. It should also integrate effortlessly with existing Electronic Medical Records (EMR) and practice management systems to minimize administrative workload [16,20,22].
A great example is the AIH Health App, which connects wearable devices like the aiSpine posture monitor and aiRing vital signs tracker. These tools provide real-time health data and personalized feedback while ensuring HIPAA compliance and maintaining necessary Business Associate Agreements. The platform also generates exportable, timestamped reports of device usage for audit purposes [16,18,22].
Platforms should automatically track both monitoring days and treatment management minutes to ensure accurate billing under the 2026 code tiers [18,22]. For instance, in 2024, Athletico Physical Therapy implemented an RTM program that combined digital home exercise programs with remote monitoring. This initiative led to over 30% improvements in pain and function outcomes. Choosing a platform that can adapt to specific therapy goals and scale with practice size is essential [16,20]. The AIH Health App demonstrates how customizable platforms can support tailored therapy plans and streamline the integration of digital tools.
How to Develop Custom Wearable Device Protocols
Creating a custom Remote Therapeutic Monitoring (RTM) protocol requires a structured approach that prioritizes patient needs. The process typically involves three main steps: evaluating patient requirements, selecting suitable devices, and tailoring the protocol to align with clinical objectives and billing standards.
Assessing Patient Needs and Therapy Goals
To develop effective protocols, start by focusing on the specific needs of patients, particularly those with musculoskeletal or neurological conditions that require consistent monitoring between clinic visits.
For musculoskeletal cases, it’s important to track key metrics such as range-of-motion progress, adherence to home exercise programs, and activity completion rates. For instance, if a patient recovering from a rotator cuff surgery experiences a noticeable decline in movement consistency over three days, this could indicate a need for immediate clinical intervention.
Set clear and measurable therapy goals from the outset. Are you working to restore a specific range of motion? Improve the ability to complete certain tasks? Reduce pain during daily activities? Your monitoring plan should directly reflect these objectives. Additionally, make sure the interface is user-friendly, especially for patients who may not be tech-savvy.
"RTM is not automated care. It becomes a skilled service when the therapist reviews RTM data, interprets functional trends, documents clinical reasoning, and adjusts the plan of care." – HelloNote Expert
Selecting the Right Wearable Devices
Once therapy goals are established, choose devices that integrate effectively with digital health platforms. Focus on FDA-compliant devices that capture therapy-specific data, as consumer-grade wellness trackers may not meet the necessary standards.
For example, devices like the aiSpine are ideal for posture therapy, offering real-time tracking and reminders. Meanwhile, the aiRing provides a more comprehensive solution by monitoring vital signs alongside functional activity, making it suitable for multi-faceted therapy needs. Both devices work seamlessly with the AIH Health App, ensuring secure data export for billing and audit purposes while maintaining HIPAA compliance.
Ease of use is another critical factor. Devices should be straightforward enough for patients to use independently after initial training. Features like Bluetooth connectivity for automatic data updates, long battery life (at least seven days), and durability for everyday wear are essential.
Protocol Customization and Implementation
Tailor the monitoring frequency based on billing codes such as CPT 98977 (16 days per 30-day period) or CPT 98985 (2–15 days for short-term therapy).
Set up specific alert thresholds tied to important clinical decisions. For example, alerts could be triggered if a patient reports a two-point increase in pain levels, skips three consecutive exercise sessions, or shows signs of overexertion that might lead to re-injury. These alerts should integrate directly into your Electronic Medical Records (EMR) system to aid documentation and therapeutic decision-making.
During the initial setup (billable under CPT 98975 at $21.71), explain to patients what data will be monitored and how it supports their recovery. This step is crucial – patients who understand the purpose of monitoring are more likely to stick with the program. To meet treatment management billing requirements, schedule at least one live interactive session monthly.
Improving Patient Engagement and Protocol Adherence
Once the protocol is set up, the real challenge lies in keeping patients engaged. Without active support, adherence to home exercise programs tends to drop. Success often hinges on how well patients are educated, how consistent communication is, and how effectively technology is used to provide personalized feedback.
Educating Patients on Device Use
Patient education starts with the initial setup session, which is a billable service under CPT code 98975. This session lays the groundwork for adherence. Considering that 80% of in-clinic information is quickly forgotten, it’s crucial to reinforce instructions through digital follow-ups.
Plan a setup call once the device is delivered. During this call, guide patients through the essentials: charging the device, syncing it via Bluetooth, and understanding how the data relates to their recovery. For devices like the aiSpine or aiRing, demonstrate features such as vibration reminders and explain what activates them. Use tools like photos and videos to confirm correct device usage and proper exercise performance.
Simplicity is key. Devices with user-friendly interfaces and automatic data syncing minimize the learning curve, especially for patients who may not be tech-savvy. For example, the AIH Health App offers visual dashboards that make it easy for patients to monitor their progress. With this foundation, ongoing communication becomes the next step to sustaining engagement.
Maintaining Regular Communication
After the initial education, regular interaction is critical. As Karen Sartin, MS, CCC-SLP, Product Analyst at Net Health, puts it:
"The therapeutic relationship thus becomes strengthened as trust is established and investment in the patient’s success is demonstrated".
To meet CMS billing requirements for RTM treatment management (codes 98979, 98980, 98981), at least one live, interactive communication – via phone or video call – is required each month. While texts and emails are handy for quick updates, they don’t fulfill this requirement. Use these monthly calls to review data trends, clarify instructions, and make necessary adjustments to the care plan based on monitoring results.
Ongoing communication outside of clinic visits provides social support and immediate feedback, which are crucial for adherence. For example, in March 2026, Athletico Physical Therapy implemented Remote Therapeutic Monitoring to track patient progress and offer real-time feedback. This approach led to over a 30% improvement in pain and functional outcomes for patients using RTM.
Smartphone reminders and app notifications can also help combat forgetfulness. When patients know their therapist is actively monitoring their activity data, they’re more likely to stay engaged.
Using AI for Personalized Feedback
AI-powered devices elevate patient engagement by turning passive monitoring into active support. Devices like the aiSpine and aiRing use AI algorithms to analyze continuous data and provide tailored guidance based on each patient’s health status. Real-time vibration reminders nudge patients to correct their posture or adjust activities without requiring constant input from clinicians.
AI virtual assistants add another layer of support, available 24/7 to answer common questions about exercises, pain levels, or therapy goals. Automated alerts can flag potential issues – like missed exercise sessions or a noticeable increase in pain – allowing therapists to intervene early, before small problems escalate. These AI tools help therapists refine treatment plans using real-time, detailed insights.
The AIH Health App’s interactive dashboards let patients track their progress over time, making their goals feel more tangible. This transparency encourages a sense of autonomy and deepens the patient-provider connection – both essential for successful remote therapeutic monitoring with wearable devices.
As Karen Sartin emphasizes:
"Frequent review of this data then allows the therapist to fine-tune therapeutic programming, reinforce target behaviors, and keep the patient engaged throughout the course of care".
Using RTM Data to Improve Treatment Plans
The real value of remote therapeutic monitoring (RTM) lies in how the collected data is used. Raw numbers alone don’t drive better outcomes – it’s the thoughtful interpretation and application of that data that makes the difference. Therapists play a key role here, reviewing RTM data, identifying trends, documenting their clinical reasoning, and refining care plans to transform data into actionable, evidence-based interventions.
Identifying Trends and Barriers
RTM data helps uncover changes in patient performance that might otherwise go unnoticed. For example, it can highlight functional declines such as inconsistent movement patterns, missed home exercise days, or reduced participation after a pain flare-up or disruption in routine. This data bridges the gap between what happens during clinic visits and a patient’s daily life at home.
It’s also crucial to differentiate between lack of activity and lack of device use. Setting a minimum wear-time threshold ensures the data is reliable and prevents misinterpreting non-use as a lack of progress.
RTM can even serve as an early warning system for complications. For instance, a sudden drop in daily step counts might signal post-surgical issues like infections, delayed wound healing, or blood clots – problems that might not be visible during a routine checkup. Friedrich Lämmel, CEO of Thryve, emphasizes:
"With RTM, recovery becomes measurable in real time, giving providers early visibility into a patient’s progress. They can identify deviations from expected recovery patterns… which often precede complications".
In a January 2026 feasibility study, researchers monitored 67 Parkinson’s Disease patients using iPhones and Apple Watches over 55 days post-implant. By tracking daily fluctuations with the Patient Global Impression of Severity (PGIS), clinicians saw mean PGIS scores improve from 4.4 at baseline to 3.2 after three months. This allowed them to confirm the effectiveness of Deep Brain Stimulation therapy through both subjective surveys and wearable data. Combining these two data sources gives a fuller picture of a patient’s progress.
It’s worth noting that RTM requires at least 16 days of data within a 30-day period to meet CMS billing requirements. This ensures there are enough data points to identify meaningful trends rather than reacting to short-term fluctuations.
Adjusting Therapy Goals and Protocols
Once trends are identified, therapists can adjust treatment plans to better align with a patient’s needs. RTM data serves as a guide for modifying interventions, whether that means tweaking the intensity, frequency, or type of home exercises based on how a patient is responding.
For example, Athletico Physical Therapy implemented Limber Health’s RTM platform in March 2026 for musculoskeletal patients. The results? A 30% improvement in pain and functional outcomes compared to patients not using RTM, and those using the system completed 3.3 times more home exercise sessions than those on standard programs.
Setting alert thresholds can also help therapists respond quickly. If a patient’s pain score jumps by more than 3 points, it’s a signal to check in immediately. Conversely, if data shows a patient is easily completing level 1 exercises without pain, it might be time to progress to more advanced tasks.
Clear documentation of clinical reasoning is essential. When adjusting therapy goals, explicitly connect the changes to the RTM data. As noted in FairPath’s RTM Operator Guide:
"The more explicitly you connect RTM data to care-plan changes, the stronger your position in an audit".
Scheduling monthly live sessions to review data insights can also be beneficial. These meetings allow therapists to address barriers early. For instance, if the data shows low engagement, it’s worth investigating whether the issue is due to a lack of technological literacy rather than physical limitations. Providing extra training on device use can make a big difference.
Tools like the AIH Health App dashboard simplify the process by consolidating key metrics – such as range of motion trends, repetition counts, and pain scores – into one place. This streamlined view makes it easier to spot patterns and adjust protocols without getting overwhelmed by data. With studies showing that 300 patients wearing Apple Watches for three months generated 6 million kilobytes of data, having summarized metrics is critical.
| Data Signal | Identified Barrier | Protocol Adjustment Action |
|---|---|---|
| Low Exercise Completion | Lack of time or tech literacy | Simplify HEP or provide device training |
| High Pain Scores during ROM | Exercise too intense | Reduce reps or modify movements |
| Rapid Goal Achievement | Protocol too easy | Progress to higher-level tasks |
| Frequent "Rescue" Events | Environmental triggers | Increase education and check-ins |
Conclusion: The Future of Remote Therapy Monitoring in Occupational Therapy
Remote therapeutic monitoring (RTM) is changing how occupational therapists provide ongoing, data-driven care. By leveraging wearable devices and platforms powered by AI, therapists are seeing impressive results – patients using RTM complete 3.3 times more home exercise sessions and experience over a 30% improvement in pain and functional outcomes.
The financial framework is also adapting to make RTM more accessible. Starting in January 2026, new CMS billing codes (CPT 98985 and 98979) will allow therapists to bill for just 2 days of monitoring and 10 minutes of management. With musculoskeletal conditions costing the U.S. healthcare system $600 billion annually, this early intervention approach offers both clinical and economic benefits. Additionally, the rise of value-based care models, such as the Merit-Based Incentive Program (MIPS), highlights how RTM data can support both improved patient outcomes and financial sustainability. Therapists who use RTM insights to guide their clinical decisions and adjust treatment plans can demonstrate measurable improvements, strengthening their practice in the long term.
Looking ahead, advanced analytics and device flexibility are key to RTM’s evolution. AI and predictive tools will help therapists identify digital biomarkers – like subtle changes in movement or gait – before they escalate into clinical issues. Moreover, platforms are increasingly compatible with consumer devices like Apple Watches and Fitbits, making it easier for patients to engage with these tools while syncing data directly to clinical dashboards. This adaptability lowers barriers to adoption and aligns with patients’ preferences, further boosting RTM’s potential to transform care.
Custom RTM protocols take monitoring to the next level by turning data into actionable insights. When therapists review RTM data, interpret trends, document their clinical reasoning, and adjust care plans, monitoring becomes a skilled therapeutic service. These tailored approaches not only enhance outcomes but also allow therapists to deliver personalized care efficiently. With technology enabling this patient-focused approach, RTM is set to redefine the future of occupational therapy.
FAQs
What makes an RTM app qualify for billing?
An RTM app becomes eligible for billing when it utilizes FDA-recognized medical devices or approved Software as a Medical Device (SaMD) to gather non-physiologic data related to therapy adherence and response. To qualify, it must clearly document therapy versus non-therapy routines, meet required device-day thresholds, include live management interactions, and provide accurate timestamps. These elements ensure the app aligns with CMS and payer-specific regulations.
How do I choose the right wearable for a patient?
When choosing a wearable for remote therapeutic monitoring, start by considering the patient’s specific therapy goals and the health metrics that need to be tracked, such as movement, posture, or vital signs. Look for FDA-approved devices specifically designed for medical purposes. Options like AIH LLC’s aiSpine or aiRing are excellent examples, as they seamlessly integrate with the AIH Health App.
It’s equally important to ensure the device offers secure data collection, fits well with the therapy plan, and provides features like real-time tracking and personalized feedback to support the patient’s progress effectively.
What alert thresholds should an RTM protocol include?
An RTM protocol needs to establish alert thresholds by analyzing data collected for a minimum of 16 days within a 30-day timeframe. Additionally, it should outline management time thresholds, typically ranging from 10 to 20 minutes per month, to guarantee efficient monitoring and prompt action when necessary.