AI is transforming Electronic Health Record (EHR) systems by automating clinical documentation and reducing administrative burdens. Physicians spend nearly 6 hours daily on EHRs, leading to burnout. AI tools like ambient documentation and voice-first assistants are helping streamline workflows, save time, and improve patient interactions. Here’s how leading EHR platforms are leveraging AI:
- Epic Systems: Fully integrated AI tools like "AI Charting" reduce after-hours documentation by 26% and save 34 minutes daily. Features include voice commands and real-time note generation.
- Oracle Health (Cerner): Voice-powered Clinical AI Agent cuts documentation time by 30%. It’s active across 30+ specialties and drafts orders alongside notes.
- Allscripts: Partners with Dragon Medical One for voice commands and transcription, saving 2–3 hours daily and reducing claim denials by 40%.
- athenahealth: Offers athenaAmbient, a digital scribe included at no extra cost, generating encounter notes instantly and reducing after-hours workload.
These platforms prioritize integration, accuracy, and efficiency, addressing the specific needs of clinicians and practices.
1. Epic Systems
Documentation Automation
Epic’s AI Charting, part of its Art suite, simplifies documentation by transforming real-time conversations between patients and clinicians into clinical notes and queuing orders directly within the system. Unlike third-party tools that overlay on electronic health records (EHRs), this AI is fully integrated into Epic’s platform, utilizing the complete longitudinal medical record for context-based documentation.
In February 2026, Group Health Cooperative of South Central Wisconsin became the first to implement AI Charting. Dr. Kate Ledford, one of the clinicians using the tool, shared how it transformed her workflow:
"It’s changed my life and made note‐writing so much easier. It’s saving me time, which is great, but it’s also saving my sanity and allowing me to give more attention directly to my patients".
Clinicians can even use voice commands to customize formatting, such as turning the history of present illness into a bulleted list.
The benefits extend beyond physicians. For example, nurses at Mercy Health System cut end-of-shift documentation time by 85%, reducing it from 3.5 minutes to just 32 seconds per note, while also achieving a 225% boost in on-time note completion. Additionally, Epic’s "Penny" AI agent assists with billing by suggesting Level of Service codes based on free-text notes, leading to 20% fewer coding denials.
All this is supported by Epic’s robust and secure data exchange protocols, ensuring smooth integration across workflows.
Interoperability
Epic leverages SMART on FHIR and OAuth 2.0 protocols to connect with external AI engines. Through the FHIR Observation resource, the system seamlessly incorporates data from health monitoring devices and wearables, such as vitals and flowsheet information. MyChart Central further enhances this by providing patients with a unified Epic ID across all 50 states, allowing AI tools to access a comprehensive medical record .
Epic also actively participates in TEFCA (Trusted Exchange Framework and Common Agreement) and was one of the first platforms to share medical records with the Social Security Administration, ensuring continuous AI integration across care settings. This interoperability extends to AI-powered wearable devices, including those from AIH LLC, which monitor spine health and chronic conditions.
Efficiency Gains
Epic’s integrated tools aren’t just about documentation – they also deliver measurable efficiency improvements. By early 2026, 85% of Epic customers had adopted generative AI tools across the Art, Emmie, and Penny suites. Clinicians using AI Charting reported a 26% drop in after-hours documentation time. At Riverside Health in Virginia, Art’s Inpatient Insights tool reduced time spent on documentation and communication tasks by 32%, while discharge summaries were completed 20–30% faster using the "Draft Hospital Course Notes" feature.
The "Insights" summarization tool, which compiles patient history and recent notes into pre-visit summaries, is now used more than 16 million times monthly as of February 2026. At John Muir Health, ambient listening technology saved clinicians 34 minutes daily on note-writing, contributing to a 44% reduction in physician turnover. Corey Miller, Epic’s Vice President of R&D, emphasized the transformative impact of these tools:
"AI Charting represents a real opportunity to change the lives of all the clinicians using our software… we view Art as an active assistant throughout the patient visit".
These advancements directly address the growing issue of clinician burnout, easing administrative burdens and allowing healthcare professionals to focus more on patient care.
sbb-itb-44aa802
2. Cerner (Oracle Health)
Documentation Automation
Oracle Health’s Clinical AI Agent integrates voice-first technology into its cloud-based EHR system. By using ambient listening, it captures conversations between patients and providers in real time and generates draft clinical notes within minutes. Unlike basic transcription tools, it employs semantic reasoning to align medications with diagnoses for more accurate documentation.
In March 2025, Southwest General Hospital in Middleburg Heights, Ohio, implemented the Clinical AI Agent across several specialties. Jacqulyn Stachowiak, CNP, praised the system for filtering out irrelevant side conversations while capturing crucial medical details, enabling her to concentrate fully on her patients.
"I am able to have good conversations with my patients, obtain a detailed history and not have a mental burden to remember everything I said during the encounter."
- Dr. Mujtaba Mohamed, Marshall Health
The tool also drafts clinical orders – such as lab tests, imaging, prescriptions, and follow-ups – for provider review, streamlining the entire process. By March 2026, Oracle expanded the AI Agent’s capabilities to over 30 specialties, covering ambulatory, inpatient, and emergency departments.
This automation also sets the stage for seamless integration with external devices and systems.
Interoperability
Oracle Health’s interoperability features build on its documentation automation capabilities, utilizing FHIR® R4 APIs and the SMART on FHIR framework for third-party integrations. It supports over 90 FHIR resources for both reading and writing operations, ensuring compatibility with a wide range of systems. For example, wearable devices from AIH LLC, which monitor spine health and chronic conditions, feed structured data directly into the EHR using FHIR Observation resources. Authentication is handled securely via OAuth 2.0.
The platform includes a centralized interoperability management console for clinical data exchange, which has driven an 85% clinician adoption rate for AI tools – compared to just 48% for simpler, text-only integrations. Oracle has also applied to become a Qualified Health Information Network (QHIN) under TEFCA, aiming to enhance nationwide data sharing capabilities.
Efficiency Gains
Clinicians using the Clinical AI Agent report a 30% reduction in daily documentation time. Within its first year in the U.S., the system saved doctors over 200,000 hours of documentation work.
Following a successful pilot, AtlantiCare in New Jersey rolled out the Clinical AI Agent across all its emergency departments in March 2026. CIO Jordan Ruch highlighted the transformative impact:
"When documentation becomes lighter and more intuitive, it changes the dynamic of a shift. Our providers can stay present with patients instead of thinking about the screen."
- Jordan Ruch, CIO, AtlantiCare
At Billings Clinic – Logan Health, Dr. Randy Thompson, Chief Health Analytics Officer, noted that automation significantly improved work–life balance for staff by reducing the paperwork burden in high-pressure environments. The system slashes note finalization time by 65–75% and reduces the time spent on documentation from 12–15 minutes per note to just 30–90 seconds. These improvements not only streamline workflows but also allow clinicians to dedicate more time to patient care, enhancing the overall clinical experience.
3. Allscripts
Documentation Automation
Allscripts is making strides in reducing clinician workload by introducing voice-operated documentation tools. Through partnerships with Microsoft and Nuance, it integrates AI-powered solutions like Dragon Medical One and Dragon Copilot. These tools go beyond basic transcription by using speech recognition to capture ambient clinical conversations and automatically convert them into structured clinical notes.
With voice-command shortcuts, providers can quickly handle repetitive tasks or insert detailed text blocks. For instance, at Singing River Health System, these tools saw an impressive 88% adoption rate, with clinicians using around 22,000 voice commands monthly to simplify their workflows.
"One of the things that’s helped providers, including myself, become more efficient and save even more time with Dragon Medical One are the shortcuts that do repetitive actions a lot faster than finding and clicking on things or typing in long paragraphs of text."
- Dr. Clinton Hull, Medical Director of Clinical Informatics, Singing River Health System
Adding to this, the PowerMic Mobile feature transforms smartphones into secure wireless microphones, enabling remote access for documentation tasks.
These documentation capabilities are further strengthened by Allscripts’ focus on seamless data exchange.
Interoperability
Allscripts employs FHIR APIs and HL7 messaging to facilitate smooth, bidirectional data flow. This allows tools to pull critical patient information – like medical history and medications – and write back structured data, such as ICD-10 codes and CPT mappings. By ensuring secure data sharing through FHIR APIs, Allscripts helps unify information across different platforms and devices, enhancing clinical decision-making.
In remote monitoring scenarios, devices like those from AIH LLC can transmit data on spine health and chronic conditions directly into Allscripts platforms. This process is supported by secure OAuth 2.0 authentication, ensuring data integrity across connected devices.
Efficiency Gains
Allscripts’ ambient documentation tools save providers an estimated 2–3 hours per day, with an 85% reduction in note finalization time.
Beyond documentation, the integration with Dragon Medical One and Dragon Copilot automates several administrative tasks. For example:
- Benefits verification: Reduced from 15–20 minutes per patient to instant checks.
- Prior authorizations: Turnaround times improve from days or weeks to same-day approvals.
- Billing and claims: AI tools decrease claim denials by 40%, recovering $50,000–$200,000 in lost revenue per provider annually.
"This is the first time in my career I’ve ever seen a suite of technologies that our providers actually want and ask for."
- Philip Payne, Chief Health AI Officer, BJC Health System
These advancements not only save time but also streamline workflows, paving the way for more innovations in healthcare technology.
4. athenahealth
Documentation Automation
athenahealth is rolling out athenaAmbient, an integrated digital scribe within athenaOne. This tool listens to clinician-patient conversations during both in-person and telehealth visits, generating encounter notes, diagnoses, and prescriptions within seconds after the visit ends. The best part? athenaAmbient will be included in routine updates for athenahealth customers at no extra charge.
With additional features like Sage and Clinical Inferences, clinicians can quickly access patient history and identify care gaps, ensuring encounters are thorough and meet billing requirements.
"With our new AI-native clinical encounter, we’re ushering in a new era where technology fades into the background. It listens to the visit, understands the context, and engages in real time – so clinicians can focus on what truly matters: the patient."
- Bob Segert, Chairman and CEO, athenahealth
athenaAmbient began user testing in February 2026, with broader AI-native clinical encounter testing planned for the first half of 2026. These tools pave the way for smooth data exchange through an intelligent interoperability framework.
Interoperability
In addition to its documentation tools, athenahealth enhances data flow with advanced interoperability features. The ChartSync engine consolidates data from external EHRs, payers, and registries, presenting a chronological "Changes since last visit" summary. During alpha and beta testing, 90% of AI-generated summaries from ChartSync were rated accurate by clinicians. This functionality helps providers focus on high-priority content, like discharge outcomes, without combing through multiple files.
The platform uses an open API architecture and the Model Context Protocol (MCP) server to standardize communication between various AI models and athenaOne. Enhanced AI reconciliation of medications and allergies saves clinicians an average of 10.6 clicks per reconciled data source. Beta testers reported an 80% boost in satisfaction with AI-powered interoperability workflows.
"The differentiator will not be who can exchange the most information, but who can make that information clear, actionable, and manageable for clinicians."
- athenahealth
For remote monitoring, devices like those from AIH LLC integrate seamlessly with athenaOne, securely transmitting data on spine health and chronic conditions via API connections. This ensures compatibility with existing workflows.
Efficiency Gains
athenahealth’s AI tools aim to tackle after-hours documentation. Family physicians currently spend an average of 86 minutes on administrative tasks after hours, a workload athenaAmbient is designed to reduce. By creating draft notes in real time, the system allows clinicians to finalize documentation immediately.
Beyond documentation, the platform automates revenue cycle management. AI predicts copays, flags the best times for claim follow-ups, and selects accurate billing codes from encounter notes. It also handles routine communications by managing inbound texts and calls, triaging common questions, and filling canceled appointment slots through its "Waitlist Scheduling" feature.
Recent statistics show that 68% of physicians have increased their use of AI for clinical documentation. Younger doctors (under 40) and those in larger practices (20+ physicians) are leading the charge in adopting these tools. This growing adoption underscores how AI is reshaping clinical workflows, aligning with trends across top EHR systems.
AI Tools for Documentation: The Newest Member of the Care Team
Pros and Cons
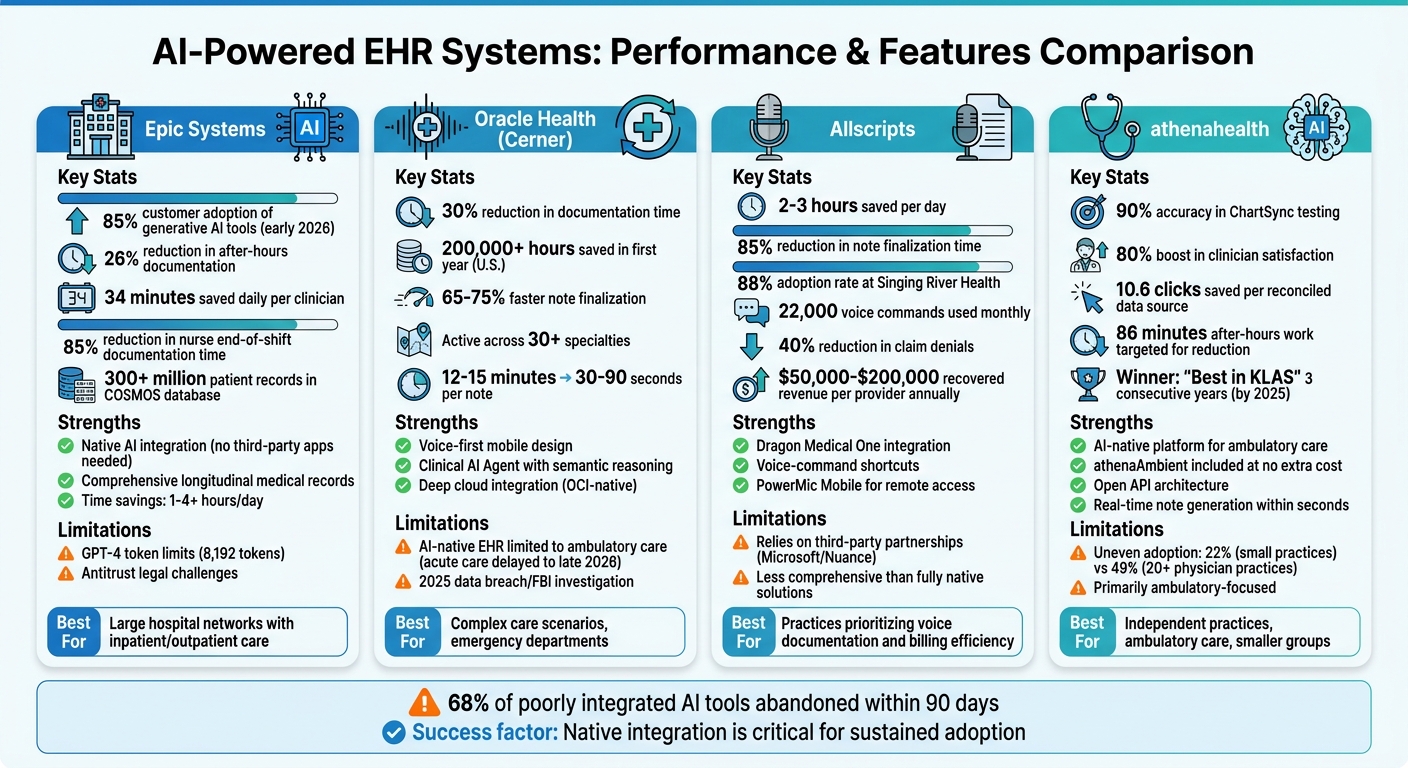
AI-Powered EHR Systems Comparison: Epic vs Oracle Health vs Allscripts vs athenahealth
Each EHR system brings its own strengths and challenges, directly influencing how effectively they integrate AI into clinical workflows. Here’s a closer look at the advantages and drawbacks of these platforms based on their AI capabilities.
Epic Systems has surged ahead, with 85% of its customers actively using generative AI tools as of early 2026. Its AI Charting tool, launched in February 2026, eliminates the need for "clipboard workarounds" often required with third-party apps. The system leverages its COSMOS database, containing over 300 million patient records, to enhance its AI models. However, Epic has faced legal challenges over antitrust concerns, and its older GPT-4 integrations sometimes run into token limits, leading to omissions in patient notes exceeding 8,192 tokens.
Oracle Health (formerly Cerner) stands out for its voice-first mobile design, thanks to the Clinical AI Agent, which is now operational across 30+ specialties. This tool has significantly reduced documentation time. However, its AI-native EHR is currently limited to ambulatory care, with acute care functionality delayed until late 2026. Additionally, a 2025 data breach led to an FBI investigation, raising concerns about security.
athenahealth has earned recognition as an "AI-native" platform for ambulatory care, winning the "Best in KLAS Overall Independent Physician Practice Suite" award for three consecutive years by 2025. Its open API architecture supports seamless integration with third-party documentation tools, and its ChartSync engine achieved 90% accuracy during testing. Despite these strengths, adoption remains uneven – only 22% of small practices use AI tools compared to 49% of larger practices with 20+ physicians.
Key Metrics Comparison
The table below summarizes the performance and features of these EHR systems:
| EHR System | Automation Accuracy | Integration Ease | Time Savings |
|---|---|---|---|
| Epic Systems | High; CoMET foundation models | Native embedding; no third-party apps needed | 1–4+ hours/day |
| Oracle Health | High; multimodal, voice-first | OCI-native; deep cloud integration | ~30% reduction in documentation time |
| athenahealth | 90% accuracy in ChartSync testing | Open API; cloud-native architecture | Varies by practice size; high in larger groups |
Key Insights
Seamless integration plays a pivotal role in ensuring AI adoption and improving workflow efficiency. Systems that rely on poorly integrated AI tools often face high abandonment rates – 68% of such tools are dropped within 90 days. Moreover, physicians emphasize that errors of omission, where critical clinical details are missing, are a bigger concern than hallucinations in AI-generated notes. These factors highlight the importance of robust, well-integrated AI solutions in modern EHR systems.
Conclusion
Selecting the right EHR system hinges on your organization’s specific needs. For large hospital networks managing both inpatient and outpatient care, Epic Systems is a strong contender. Its AI-powered Charting tool drafts notes in real time by drawing from extensive historical data, making it a valuable asset for streamlining documentation tasks.
For ambulatory care practices that value simplicity and efficiency, athenahealth shines as an AI-native option. Its athenaAmbient digital scribe, included at no extra cost, listens to patient visits, understands context, and engages in real time. As Bob Segert, Chairman and CEO of athenahealth, explains:
"With our new AI-native clinical encounter, we’re ushering in a new era where technology fades into the background. It listens to the visit, understands the context, and engages in real time".
This functionality makes athenahealth particularly appealing to independent practices and smaller groups.
On the other hand, Oracle Health (Cerner) is tailored for complex care scenarios. At AtlantiCare, the Clinical AI Agent reduced documentation time by 41%, prompting the health system to roll it out across all emergency departments by March 2026. Highlighting its impact, Jordan Ruch, AtlantiCare’s Chief Information Officer, shared:
"When documentation becomes lighter and more intuitive, it changes the dynamic of a shift. Our providers can stay present with patients instead of thinking about the screen".
Additional acute care features are anticipated by late 2026.
To ensure the best fit for your practice, conducting a pilot test is essential. Run a 2–4 week trial with a small group of clinicians to evaluate how the AI integrates into your workflow. Focus on systems with native AI integration to guarantee a smooth and tailored experience. Keep in mind that general-purpose AI models may fall short in addressing the specific needs of specialized fields like behavioral health or emergency medicine.
FAQs
How do I pilot an AI scribe in our EHR without disrupting clinic flow?
To introduce an AI scribe into your EHR system effectively, begin with a small-scale trial. This allows you to assess how well it fits into your current workflows and its overall impact. Opt for ambient AI technology that connects seamlessly with EHRs using APIs like SMART on FHIR. Before rolling it out, conduct a thorough evaluation, involve clinicians from the start, and keep a close eye on the pilot phase to resolve any challenges quickly. Taking this step-by-step approach helps maintain smooth operations while improving clinical efficiency.
What’s the best way to measure real-time savings and burnout impact after rollout?
To evaluate the real-time savings and the effect on burnout after adopting AI-powered EHR systems, it’s essential to use a mix of quantitative and qualitative metrics. For measurable data, monitor reductions in areas like documentation time, administrative workload, and hours spent working outside regular shifts. On the qualitative side, gather feedback through surveys or interviews to gauge clinician satisfaction, work-life balance, and mental strain. By blending these approaches, you’ll get a clearer picture of efficiency improvements and the impact on clinician well-being, paving the way for ongoing workflow refinements.
How can wearable data (like AIH LLC monitoring) be written into the EHR using FHIR?
Wearable data from AIH LLC devices, like the aiRing or aiSpine, can seamlessly connect to electronic health records (EHRs) using FHIR (Fast Healthcare Interoperability Resources) through secure APIs. These devices transmit structured health metrics – such as vital signs or posture data – via RESTful FHIR endpoints, ensuring smooth data flow.
Using SMART on FHIR apps and event-driven hooks, this integration allows for real-time updates to patient records. This not only reduces the need for manual data entry but also improves the accuracy of patient information and simplifies clinical workflows.