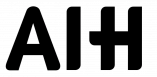Emotion-aware interfaces are transforming how we manage chronic diseases like diabetes, hypertension, and chronic pain. These systems interpret emotional cues – such as tone of voice, facial expressions, and physiological signals – to provide tailored support that addresses both physical and emotional needs. Here’s why this matters:
- Chronic Conditions and Emotions: Over half of U.S. adults face chronic illnesses, many of which are linked to mental health challenges like anxiety and depression. Yet, only 21% of AI research in chronic care focuses on emotional self-management.
- AI in Action: A 2023 study showed how GPT-4 helped a patient with critical hypertension manage stress, resulting in normalized blood pressure within 90 days.
- Technology Highlights: Combining AI algorithms, wearable sensors, and large language models (LLMs), these systems analyze emotional and physiological data to provide real-time, empathetic responses.
Examples include devices like the aiSpine (monitors posture and emotional stress) and aiRing (tracks vital signs and emotional well-being). These tools not only improve patient engagement but also enable early detection of health issues by analyzing patterns in emotional and physical data.
Emotion-aware technology bridges the gap between physical symptoms and emotional care, making chronic disease management more effective and personalized.
Ambient Intelligence & Emotion AI in Healthcare – The Medical Futurist
sbb-itb-44aa802
Technologies Behind Emotion-Aware Interfaces
Emotion-aware systems combine AI-driven emotional detection with advanced sensors to translate physiological data into actionable insights. These systems serve as a foundation for personalized chronic care solutions, which will be discussed in later sections.
AI Algorithms for Emotion Detection
Accurate emotion detection is a cornerstone of improving patient engagement. Traditional methods have been replaced by more advanced hybrid deep learning models. These models combine Convolutional Neural Networks (CNNs) to identify spatial patterns, BiLSTMs to capture temporal dynamics, and Transformers to process long-range dependencies. Together, they achieve impressive accuracy rates – up to 89.5% on benchmark datasets. Attention mechanisms further refine this process by emphasizing the most relevant signals, such as prioritizing heart rate during exercise or skin conductance during rest.
Large Language Models (LLMs) like GPT-4 enhance this capability by interpreting multimodal inputs and delivering empathetic, context-sensitive responses. Researchers at the University of Glasgow highlight the potential of LLMs in mental health applications:
"Mental health is considered a particularly suitable domain for LLMs because emotional regulation is fundamentally rooted in language."
Sensor Integration for Emotional and Physiological Data
Wearable devices play a pivotal role in detecting emotions through multimodal sensing, which combines data from physiological, visual, auditory, and behavioral inputs. Common sensors include PPG for tracking heart rate, EDA for measuring skin conductance, and accelerometers for monitoring movement. These tools provide objective insights into stress and arousal levels, offering a reliable alternative to self-reported data, which can often be inaccurate.
Research conducted at institutions like Massachusetts General Hospital, MIT, and UCSF has demonstrated the effectiveness of wearable sensors in predicting emotional distress and behavioral patterns, such as depression severity and substance cravings.
In the U.S., approximately 45% of the population uses smartwatches or fitness trackers, with adoption rates rising to 70% among Gen Z and over 50% among millennials. This widespread use creates the potential for "closed-loop" systems – devices that autonomously detect emotional or physical irregularities and respond with tailored interventions. For example, a smartwatch might send a calming notification or alert a healthcare provider, all without requiring user input.
Applications in Chronic Disease Management
Emotion-Aware Interfaces in Chronic Disease Management: Applications and Outcomes
Emotion-aware interfaces are reshaping chronic disease care by blending emotional insights with sensor-driven data. Instead of relying solely on traditional pain scales or occasional doctor visits, these systems use AI to analyze continuous, detailed data, allowing for treatments tailored to both physical symptoms and emotional well-being.
Such tools offer real-time guidance and emotional support, which is invaluable for patients dealing with physical conditions alongside anxiety or depression. For instance, digital pain coaches powered by machine learning provide personalized strategies like pacing, exercise recommendations, and cognitive-behavioral techniques through conversational platforms. Multicenter studies have shown that these approaches significantly improve pain interference, physical function, and psychological distress over 12-week periods. These advancements are paving the way for more targeted solutions in areas like spine health and pain management.
Spine Health and Posture Correction
Spine health presents a unique challenge: patients often feel better before measurable functional improvements occur. A 2022 study conducted at Ohio State University, involving the "Conity" system and 121 lumbar fusion patients, revealed that while patients reported feeling better after six weeks, objective improvements were not evident until the six-month mark.
"You simply can’t only ask people how they feel about their back." – William Marras, Executive Director of the Spine Research Institute at Ohio State
This highlights the importance of combining subjective patient feedback with objective clinical data. The aiSpine device from AIH LLC addresses this gap by tracking angular changes in the neck and back while providing emotional feedback to encourage better posture habits. Using behavioral coaching techniques rooted in nudge theory, the device helps patients overcome fear-avoidance behaviors often linked to chronic back pain. By analyzing motion patterns alongside emotional data, it can assess whether a back condition is improving, worsening, or requires further clinical attention.
Pain Management and Stress Monitoring
Emotion-aware technology also plays a key role in refining pain management and stress monitoring. These systems identify stress and pain through verbal and non-verbal cues – such as tone of voice, facial expressions, and body language – while also using sensors to track physiological indicators like heart rate variability and skin conductance.
The aiRing device combines vital signs monitoring with emotional tracking, using advanced sensors and AI algorithms to detect patterns in various situations. Paired with the AIH Health App, it provides a comprehensive view of how pain and stress interact throughout the day. This integration of emotional and physical data allows for highly personalized care, bridging the empathy gap often found in digital health solutions. Studies have shown that personalized emotional responses in these systems can increase patient engagement, with mean engagement ratios rising from 0.26 to 0.31.
| Chronic Condition | Interface Functions | Patient Outcomes |
|---|---|---|
| Chronic Pain | Activity–pain correlation; Personalized behavioral guidance | Reduced pain interference; Improved physical function |
| Cardiovascular | Remote deterioration detection; Personalized care planning | Early detection of clinical deterioration; Reduced hospitalizations |
| Respiratory (COPD) | Risk prediction; Virtual conversational agents for exacerbation support | Improved self-efficacy; Enhanced quality of life |
| Mental Health | Personalized emotional support; Triage and self-monitoring | Increased user satisfaction; Better mood management |
These examples show how emotion-aware interfaces go beyond simply collecting data. They actively provide intelligent, adaptive support tailored to each patient’s unique needs. By combining predictive analytics with empathetic feedback, these systems empower patients to develop healthier habits while equipping clinicians with actionable insights for more effective care.
Integration with AIH LLC Devices
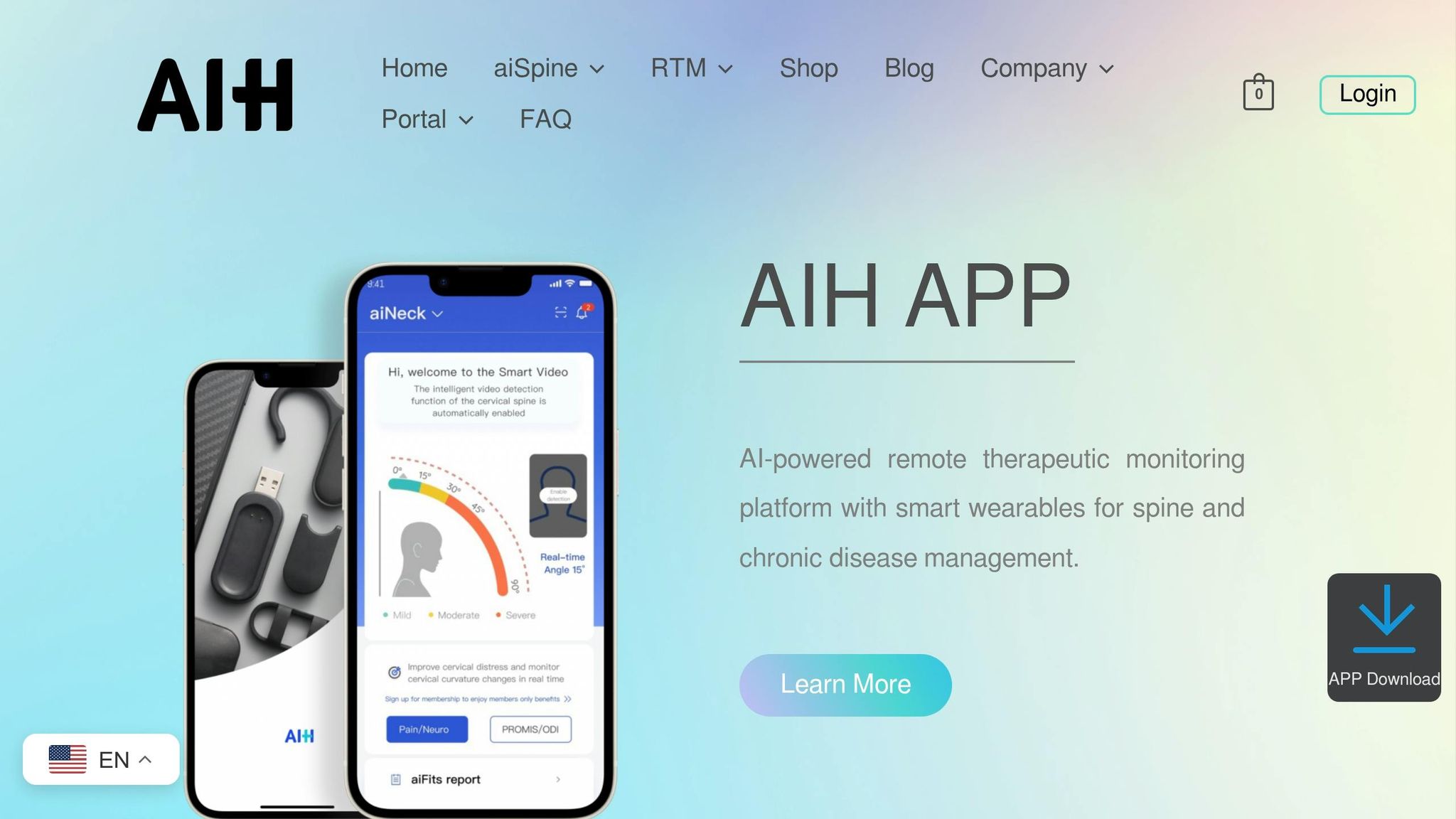
AIH LLC’s devices combine advanced sensor technology with emotion-aware capabilities to redefine chronic care. The aiSpine, aiRing, and AIH Health App work seamlessly to gather physiological and emotional data, offering a more complete understanding of a patient’s overall well-being – far beyond traditional health metrics.
aiSpine: Tracking Posture and Emotional Signals
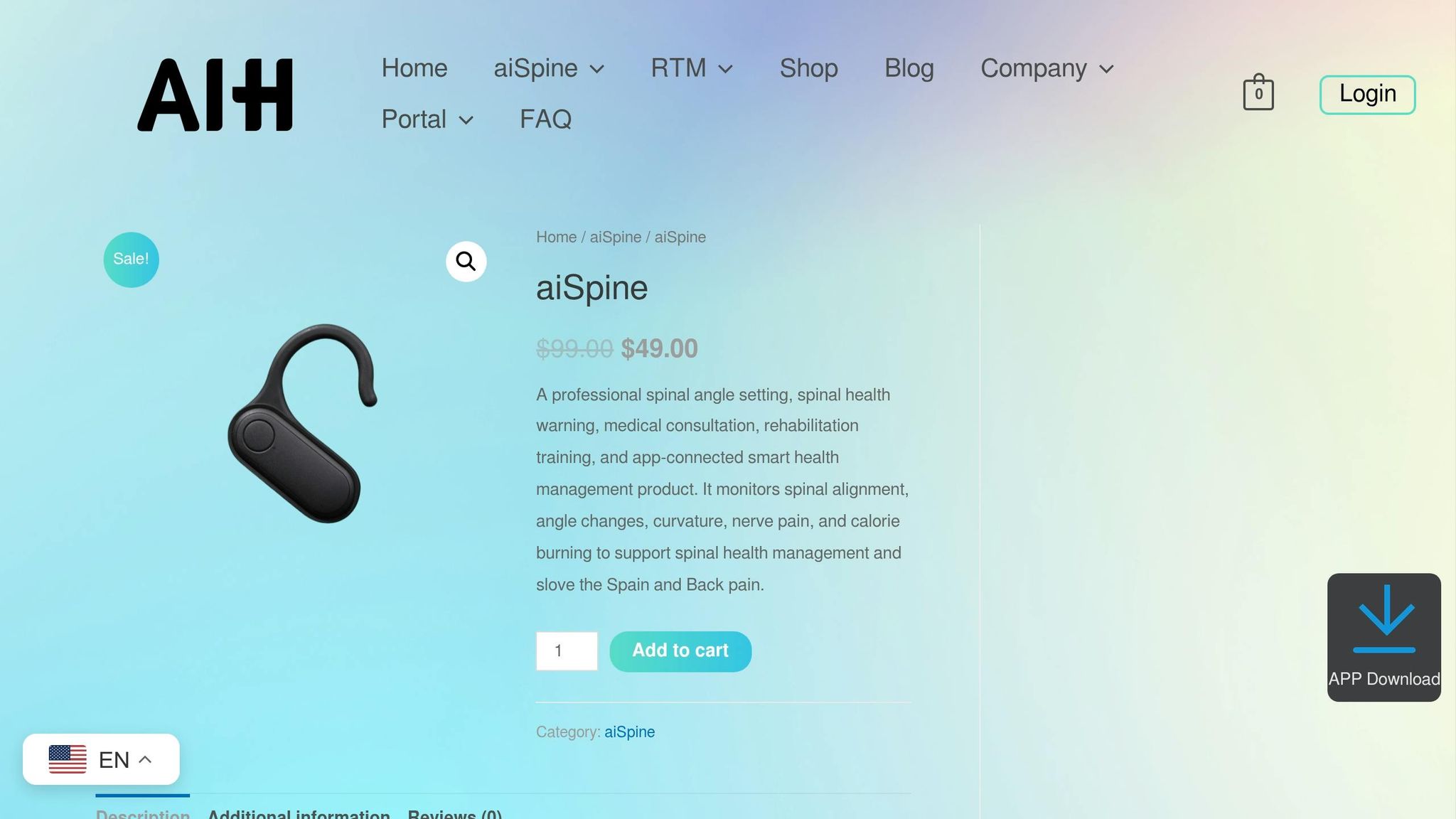
The aiSpine monitors spinal alignment while also detecting emotional stress linked to poor posture. This dual-purpose device doesn’t just focus on physical alignment – it also interprets how posture changes might reflect emotional distress.
To encourage consistent use, the aiSpine offers flexible mounting options. If it detects poor posture or stress-related patterns, it provides gentle vibration reminders to help users adopt healthier habits. While the aiSpine focuses on posture, its companion device takes on the critical task of monitoring vital signs.
aiRing: Vital Signs and Emotional Monitoring
The aiRing builds on the data gathered by the aiSpine, honing in on vital signs and emotional well-being. By tracking heart rate variability (HRV) and sleep patterns – key indicators of emotional health – the aiRing can identify early signs of emotional distress and alert clinicians for timely intervention. Its discreet touch controls make it easy to use without drawing attention, while continuous monitoring ensures vital health data is captured throughout the day.
AIH Health App: Centralized Emotional Support
The AIH Health App acts as the command center, integrating data from both the aiSpine and aiRing into actionable insights. As an AI-powered Remote Therapeutic Monitoring (RTM) platform, it combines physiological data, posture metrics, and even self-reported inputs from patients. This approach delivers a full picture of how physical and emotional states interact.
"AIH LLC provides systematic smart wearable products created and developed by medical experts while offering a personalized digital health management and monitoring service." – AIH LLC
What sets the app apart is its emotional response system, which adjusts feedback based on detected emotional states. For instance, if stress is identified – whether through an elevated heart rate or poor posture – the app offers immediate support, such as calming reassurance or tailored recovery recommendations. This real-time adaptability ensures the app not only tracks data but actively helps users manage their emotional and physical health simultaneously.
Benefits of Emotion-Aware Interfaces for Chronic Care Patients
With advanced sensors and AI-driven emotional analysis, emotion-aware interfaces are transforming chronic care management. These systems go beyond tracking physical health metrics – they actively respond to emotional cues, creating a more holistic approach to care. By addressing both physical and emotional needs, they provide a more supportive experience for patients managing long-term conditions.
Improved Patient Engagement
Real-time emotional feedback helps keep patients engaged with their care routines. For example, if a system detects frustration or discouragement, it can shift its tone, offering encouraging messages instead of just presenting data. Research shows that empathetic feedback – like motivational messages during stressful moments – can improve patient engagement and reduce treatment non-adherence by up to 35%. This consistent engagement leads to better health outcomes for those managing chronic conditions.
Personalized Therapy Plans
Emotion-aware systems adapt care plans based on both emotional and physical data. For instance, if a patient’s anxiety spikes alongside a rise in blood pressure, the system might suggest calming activities like deep breathing exercises. It can also simplify interfaces during critical moments. One study highlighted a diabetes app that limits non-essential features during hypoglycemic episodes, providing quick access to emergency contacts to reduce stress and improve safety. These targeted adjustments ensure patients can act quickly and effectively when it matters most.
Early Interventions Through Predictive Analytics
By analyzing patterns in mood and physiological data over time, emotion-aware systems can detect early warning signs of potential health issues. For example, changes in speech patterns or increased verbal hesitation might signal emotional distress before physical symptoms appear. When such signs are identified, the system can initiate supportive actions, like suggesting guided meditation or notifying clinicians for timely intervention.
"By identifying emotional distress early, emotion-aware AI can help prevent more severe mental health issues or complications." – Meegle Affective Computing
This approach prioritizes prevention over reaction, catching problems early when they are easier to manage. It also integrates seamlessly with remote monitoring tools, allowing healthcare providers to stay ahead of potential crises.
Remote Monitoring and Provider Collaboration
Emotion-aware interfaces play a crucial role in bridging the gap between clinical visits. By sharing emotional and physiological trends with healthcare teams, these systems provide a more comprehensive view of a patient’s condition. During virtual consultations, they can analyze vocal tone and facial expressions to give clinicians real-time insights into a patient’s emotional state. This "dual-layered view" of physical and emotional health enhances clinical decision-making.
Automated alerts further support care by notifying clinicians or caregivers of emotional triggers or behavioral changes, ensuring timely interventions without requiring constant manual oversight. Considering that chronic diseases account for 74% of global deaths annually, these tools allow healthcare providers to manage larger patient populations effectively while maintaining a personal touch.
Future Trends in Emotion-Aware Chronic Care
Emotion-aware technology is evolving rapidly, aiming to improve chronic care by addressing challenges in precision, trust, and personalization.
AI-Driven Predictive Analytics
Predictive digital twins are transforming how clinicians approach chronic conditions. By simulating patient-specific health scenarios, these tools allow healthcare providers to test treatment strategies before applying them in real life. For conditions like COPD or chronic kidney disease, digital twins can predict how patients might respond to changes in medication or lifestyle, reducing the need for trial-and-error adjustments.
Transparency is also becoming a key focus. Explainable AI frameworks, such as SHAP, are moving away from opaque "black-box" models. These systems clarify the reasoning behind predictions – like correlating increased heart rate variability with rising anxiety – making them easier for both clinicians and patients to understand.
"Explainable Artificial Intelligence–driven Clinical Decision Support Systems (AI-CDSS) can make daily self-management more predictive and proactive by fusing data from smartphones, wearables, and CGMs." – Frontiers in Public Health
Another trend is the rise of calibrated relational styles in AI technology. The use of AI companion apps has surged by 700% from 2022 to mid-2025. These systems are being designed to provide meaningful emotional support while avoiding over-dependence, modeling healthy social interactions.
As predictive algorithms improve, advancements in sensor technology are also pushing the limits of emotion detection.
Advancements in Multi-Modal Sensors
Next-generation sensors are building on existing multimodal capabilities to capture a broader range of emotional and physical data. Devices integrating EEG, eye-tracking, and skin conductance are becoming more sophisticated, allowing for better differentiation between physical stress (like exercise) and emotional distress (such as anxiety) – a distinction often missed by single-source data.
These technologies are paving the way for "closed-loop" systems. For example, a wearable device might detect elevated skin temperature, an increased heart rate, and shifts in facial expressions. By analyzing these signals together, the system can identify pain, frustration, or fatigue and adjust its responses in real time. Machine learning models combining data from continuous glucose monitors and wearables have already achieved 81.4% accuracy in predicting next-day hypoglycemia, highlighting the potential of integrated data sources.
Voice-first interfaces are also emerging as an effective way to enhance emotional connection. These systems analyze speech patterns – like tone, cadence, and hesitation – to detect distress in real time. For elderly patients or those with limited mobility, voice interaction provides an accessible way to interact with care platforms without navigating complex interfaces. By early 2025, nearly half (48.7%) of adults with mental health conditions reported using large language models for support. While this reflects growing trust in conversational AI, ensuring these interactions remain clinically appropriate is essential.
Together, these advancements are setting the stage for platforms like those from AIH LLC to deliver even more tailored and proactive chronic care solutions.
Conclusion
Emotion-aware interfaces are reshaping chronic care by moving beyond generic treatment protocols and instead offering personalized, data-driven interventions. These systems tap into voice patterns, facial expressions, and physiological signals to bridge the empathy gap in digital health, creating a more supportive and responsive experience for patients. By addressing both physical symptoms and emotional states, this approach ensures care feels more human and adaptive.
Platforms like those from AIH LLC – such as the aiSpine, which monitors posture, and the aiRing, which tracks vital signs – illustrate how advanced sensor technology combined with emotional intelligence can provide near-real-time risk assessments and early warnings. This combination of technical precision and emotional awareness enhances patient engagement and enables timely adjustments in care.
"Future directions focus on developing more accurate, explainable, and trustworthy AI models, better clinical integration, leveraging advanced AI for engagement to realize AI’s full potential in empowering patients and improving chronic disease outcomes." – Ying Du et al., Frontiers in Public Health
The impact of these systems goes beyond just clinical outcomes. They also address the psychological toll of chronic illness, offering personalized emotional support that can ease the feelings of isolation and disconnection often associated with patient-technology interactions. When paired with thoughtful human oversight and seamlessly integrated into clinical workflows, emotion-aware interfaces help sustain long-term patient engagement – a cornerstone of effective chronic disease management.
As predictive analytics, explainable AI, and multi-modal sensors continue to evolve, emotion-aware technology will play an even greater role in transforming chronic care. The challenge lies in ensuring these tools remain patient-centered, sensitive to cultural nuances, and smoothly embedded into existing healthcare systems. Done right, they hold the potential to significantly improve both health outcomes and the overall quality of life for patients.
FAQs
How does an emotion-aware interface tell stress from normal exercise?
An emotion-aware interface can distinguish between stress and normal exercise by examining a mix of physiological and emotional signals. This allows it to better understand the user’s emotional state and adjust its responses accordingly, providing tailored support for different scenarios.
What health actions can a “closed-loop” wearable take automatically?
Wearable devices with a "closed-loop" system can take on tasks like conducting regular depression screenings automatically. They aim to provide well-rounded care while promoting shared decision-making between patients and healthcare providers. Many of these devices come equipped with features like clinical dashboards and monitoring tools, making health management more tailored and efficient.
How is my emotional and biometric data kept private and secure?
Your emotional and biometric data is safeguarded using strict privacy measures. This includes ensuring patient confidentiality and implementing robust security protocols to protect your information. These measures are specifically designed to address privacy concerns and keep your data secure.