AI-powered wearables are transforming healthcare by predicting health issues before symptoms occur. Devices like smartwatches and rings track metrics such as heart rate, blood pressure, and oxygen levels. Machine learning analyzes this data to identify warning signs early, improving care for chronic conditions like diabetes and heart disease. These tools save costs by reducing hospital visits and offer real-time insights for better health management.
Key highlights:
- Early detection: AI models predict health risks hours or even days in advance, helping prevent critical events.
- Chronic condition support: Continuous monitoring for diseases like diabetes and hypertension.
- Cost savings: Annual savings of $2,840 per patient by reducing hospitalizations.
- Real-world examples: Devices like aiSpine (posture tracking) and aiRing (vital sign monitoring) integrate with apps for personalized alerts and trends.
Wearables are not just tracking tools – they enable smarter, faster interventions, making healthcare more efficient and accessible.
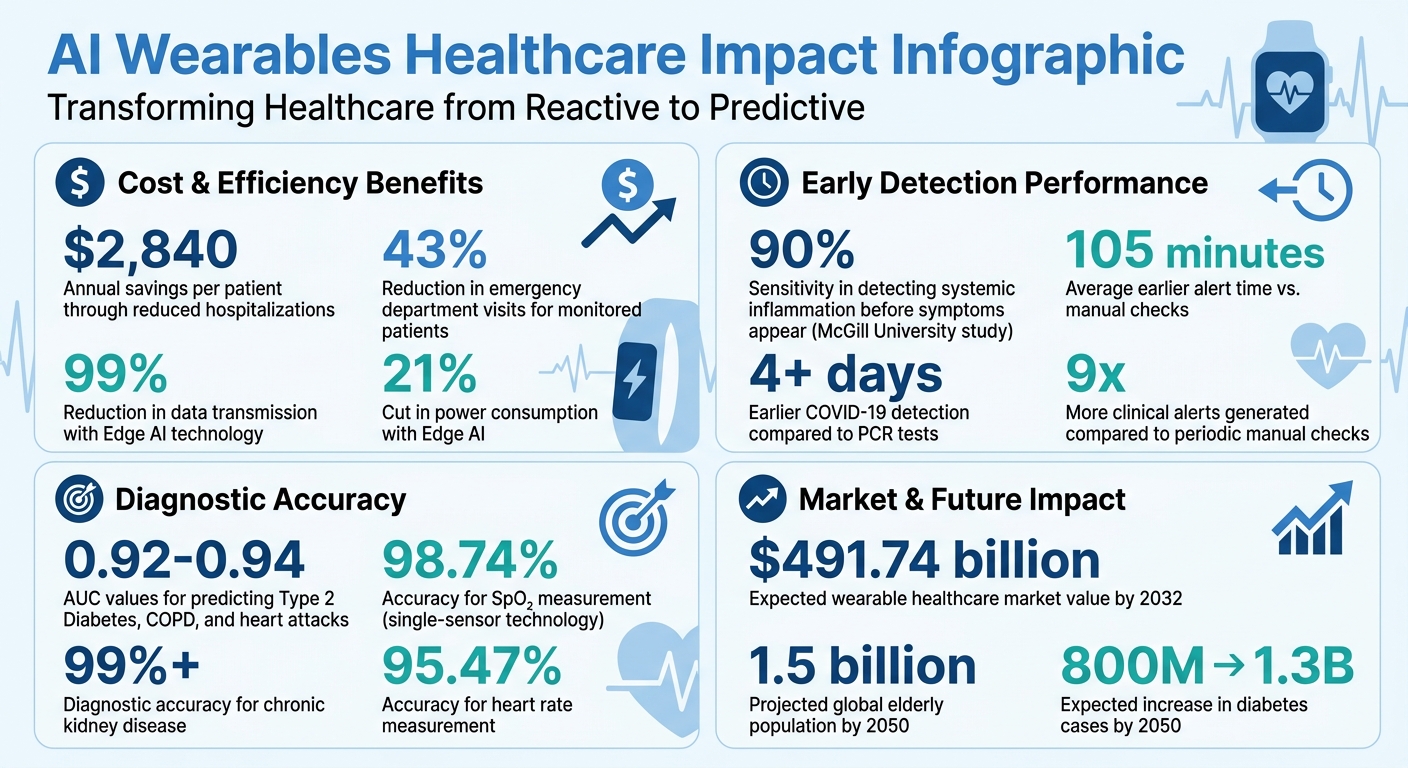
AI Wearables Healthcare Impact: Cost Savings and Early Detection Statistics
Why Predictive AI & Wearables Are Game-Changers
sbb-itb-44aa802
How Predictive Analytics Detects Symptoms Early
Predictive analytics turns raw biometric data into actionable health insights by continuously monitoring and analyzing vital signs with machine learning. Unlike the traditional hospital approach, which checks vitals every 4–8 hours, AI algorithms work in real-time. They monitor heart rate, respiratory rate, blood oxygen levels, and skin temperature, spotting subtle patterns that might signal potential health issues – often before a patient even feels unwell. This transformation of raw data into predictive insights is powered by advanced AI algorithms designed to assess specific health risks.
How AI Algorithms Predict Health Risks
AI uses advanced filtering techniques to refine data and eliminate noise. By applying methods like Moving Average and Kalman Filters, raw signals are cleaned up for analysis. From there, models such as RNN (Recurrent Neural Networks) and LSTM (Long Short-Term Memory) are employed to identify temporal trends in the data.
The real power lies in extracting complex health metrics from basic sensor data. For example, using PPG (photoplethysmography) sensors, AI can derive metrics like blood pressure and respiratory rate by analyzing waveform features such as systolic peaks and diastolic slopes. Models like Random Forest Regression, RNN, and LSTM work together to integrate real-time vitals with a patient’s historical data, creating dynamic risk profiles tailored to the individual.
Personalized baselines further improve accuracy by accounting for individual variability. This allows the system to differentiate between normal fluctuations – like those caused by exercise or caffeine – and genuine early indicators of infection or health deterioration. A notable example of this capability came in May 2026, when McGill University researchers, led by Dr. Dennis Jensen, demonstrated how their AI platform, using wearable devices like smart rings and watches, flagged systemic inflammation in 55 healthy adults. The platform identified these issues before symptoms appeared or PCR tests confirmed SARS-CoV-2 infections, achieving an impressive 90% sensitivity.
"By the time an infection is detected based on clinical symptoms or PCR testing, it is generally already well underway. Our predictive tool gives patients and healthcare providers the chance to intervene early before critical health events occur." – Dennis Jensen, PhD, Scientist, McGill University
Benefits of Early Symptom Alerts
Early detection through predictive analytics delivers real clinical advantages. By identifying risks early, healthcare providers gain the opportunity to intervene before conditions escalate. For instance, a study involving wearable smart rings showed that COVID-19 infections were detected over four days earlier than PCR tests, allowing for quicker isolation and treatment. This extra time can make a significant difference, enabling patients to receive care sooner and often avoiding severe complications.
Continuous monitoring reduces hospital visits and associated costs. Wearable devices powered by AI have been linked to a 43% reduction in emergency department visits for monitored patients. This proactive approach also brings financial benefits – sustained monitoring through wearable biosensors saves approximately $2,840 per patient annually by catching issues early and preventing costly hospitalizations. Addressing problems at an earlier stage is not only less expensive but also less stressful for patients.
For those managing chronic conditions, these alerts improve daily life. Continuous monitoring generates up to nine times more clinical alerts than periodic manual checks, thanks to the high-frequency data captured on respiratory and heart rates. When both methods detected an issue, wearables provided alerts an average of 105 minutes earlier than manual checks. This extra time can be the difference between outpatient care and an ICU visit. Patients benefit from peace of mind, knowing their devices are constantly on the lookout, while healthcare providers can focus their attention on those who need it most.
AI Wearable Technologies for Health Monitoring
AI-powered wearables are changing the game in health monitoring. These devices go beyond basic step tracking, transforming raw sensor data into meaningful health alerts. By collecting physiological data continuously, they provide a steady stream of information that AI algorithms analyze to detect early signs of potential health problems. This shift from occasional snapshots to constant monitoring means patients and clinicians can address issues before they escalate.
This transition from reactive to proactive care is reshaping health management. Continuous monitoring acts like a "check engine light" for the body, signaling when something needs attention. AI algorithms process this real-time data, integrating it with predictive models for more precise symptom tracking and intervention.
Two devices – aiSpine and aiRing – showcase how these wearables are making proactive health management a reality.
aiSpine: Posture Monitoring for Spine Health
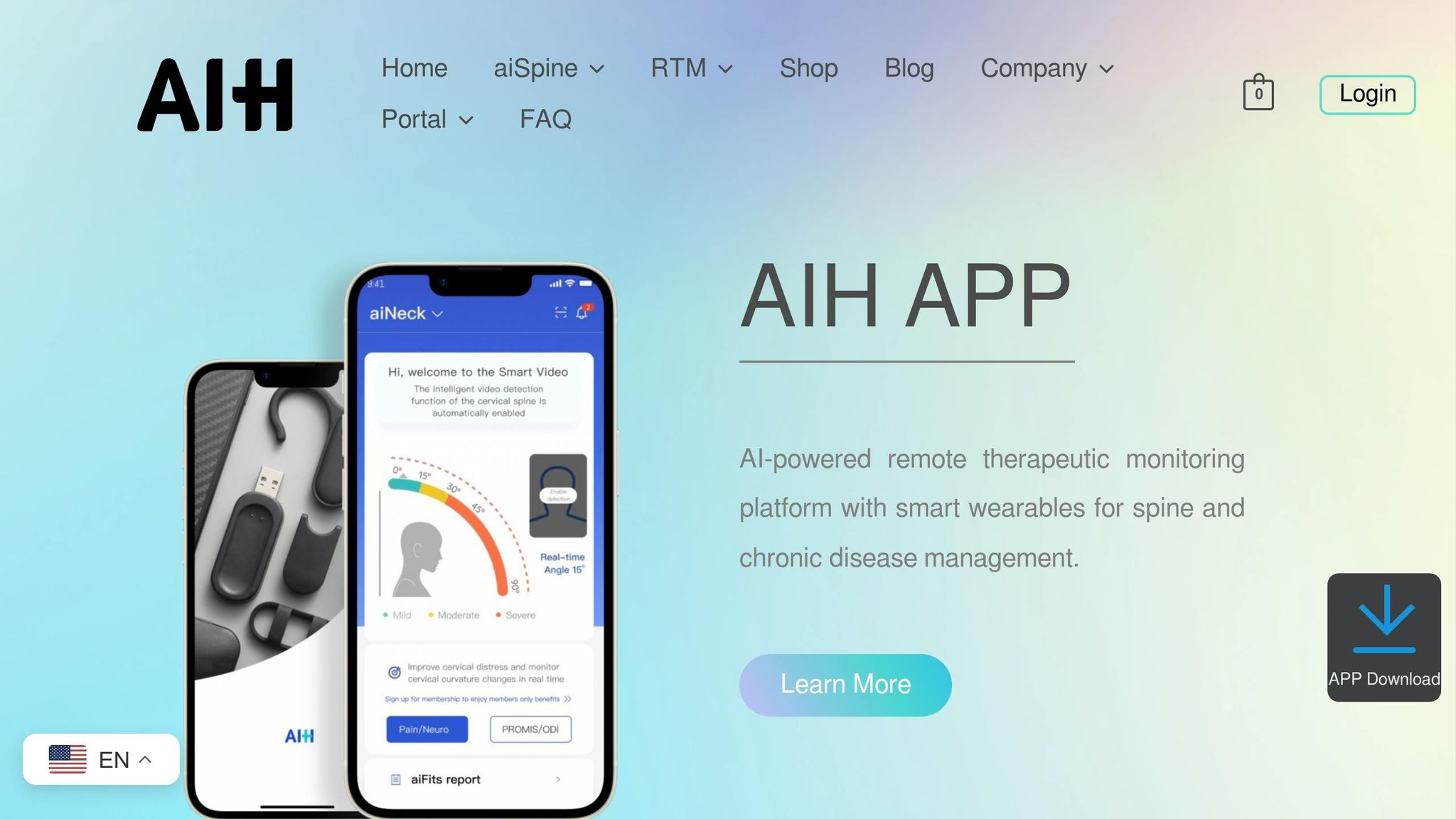
The aiSpine is designed to support spine health by tracking posture in real time. Worn throughout the day, it uses vibration alerts to nudge users into correcting poor alignment. This immediate feedback helps prevent long-term damage caused by bad posture during daily activities, offering a proactive way to manage chronic spine issues.
What makes aiSpine stand out is its connection to the AIH Health App, which records historical data and identifies patterns. Users can choose from multiple wearing modes suited to different activities, making it versatile and user-friendly. By analyzing posture habits over time, the device helps users take control of their spine health before pain or injuries develop.
aiRing: Vital Signs Monitoring for Chronic Conditions
The aiRing focuses on monitoring vital signs like heart rate, oxygen saturation (SpO₂), and body temperature to assist those managing chronic conditions. Compact and waterproof, it uses advanced sensors and AI algorithms to provide personalized, continuous tracking. For individuals with conditions such as hypertension, diabetes, or heart arrhythmias, this constant monitoring offers early warnings of potential complications.
What sets the aiRing apart is its ability to adapt to individual baselines, distinguishing normal fluctuations from potential risks. As Muhammad Manan Ali, a technology writer, explains:
"The integration of AI allows wearables to do more than just report metrics; they can recognize patterns, detect anomalies, and even forecast potential health issues before symptoms manifest."
With features like intelligent touch controls and compatibility with various scenarios, the aiRing is designed for everyday use. Its integration with the AIH Health App provides users with real-time dashboards, alerts, and long-term data trends. This turns raw sensor data into practical insights, enabling smarter self-care and better-informed decisions in collaboration with healthcare providers.
Integrating AI Wearables with Telehealth
Building on the idea of early symptom alerts, connecting AI wearables to telehealth platforms transforms raw data into actionable insights. This integration allows healthcare providers to intervene before conditions escalate. Instead of relying solely on periodic checkups or patient-reported symptoms, physicians can monitor real-time physiological changes as they happen.
The AIH Health App acts as the link between devices like aiSpine and aiRing and healthcare providers. By syncing data to cloud platforms using standards such as HL7 FHIR, low-latency 5G slicing, and Mobile Edge Computing, the app ensures uninterrupted access for providers. At the same time, advanced storage solutions and blockchain technology safeguard data integrity.
Real-Time Data Sharing with Healthcare Providers
When AI wearables integrate with telehealth platforms, they create a continuous feedback loop. These devices transmit vital signs like heart rate, oxygen levels, and temperature, enabling physicians to adjust treatments in real-time rather than waiting for the next scheduled visit. This is made possible by the Internet of Medical Things (IoMT), which connects medical devices to gather and process patient data. Apps like the AIH Health App then organize this information for clinical review. Additionally, wearables can automatically escalate alerts when they detect significant deviations from normal ranges.
Symptom Escalation Protocols for Chronic Disease Management
AI-powered wearables go beyond simple data collection – they actively monitor for dangerous patterns and issue alerts when critical thresholds are reached. For instance, if the aiRing detects irregular heart rhythms or a drop in oxygen saturation, it can notify both the patient and their care team immediately, allowing for swift intervention.
Northwell Health has already demonstrated the potential of AI in predicting patient deterioration. Their algorithms can identify life-threatening conditions, such as cardiac arrest, well in advance.
"Combining clinical wearables with the predictive AI algorithm we have developed, we can help clinicians identify these deteriorations a lot earlier and more accurately than standard-of-care early warning scores, improving patient outcomes." – Theodoros P. Zanos, PhD, Head of Northwell’s Division of Health AI
These escalation protocols use a color-coded system to prioritize responses: stable readings (dark green) are silently logged, critical states (orange) prompt immediate alerts, and emergencies (dark red) automatically notify caregivers. For chronic disease management, the AIH Health App customizes thresholds based on individual baselines, minimizing false alarms while addressing real risks promptly. This proactive approach strengthens chronic care management.
Such systems have already shown impressive results, including a 42% reduction in emergency visits and annual savings of $2,840 per patient. By supporting "hospital-at-home" models, these technologies reduce the strain on healthcare facilities while maintaining precise monitoring for conditions like heart failure, COPD, and diabetes.
The Future of AI-Driven Remote Monitoring
With advancements in telehealth, wearable technology is set to transform healthcare by shifting the focus from treating symptoms to predicting and preventing health issues before they arise. Over the next decade, these devices will play a pivotal role in proactive healthcare, moving beyond simple tracking to forecasting potential health events.
Trends in AI-Powered Healthcare Devices
One of the most exciting developments in wearables is Edge AI, which processes data directly on the device rather than relying on cloud-based systems. This approach reduces data transmission by an impressive 99% and cuts power consumption by 21%. For patients in areas with limited internet access, Edge AI ensures reliable monitoring without needing constant connectivity.
Wearable design is also undergoing a transformation. New biosymbiotic devices use 3D-printed, breathable polymer meshes that conform to the skin, replacing bulky traditional designs. These updated models enhance comfort and improve signal quality, making them more practical for long-term use. Some upcoming wearables may even feature wireless charging from distances of up to 6.5 feet and fully autonomous data logging, eliminating the need for user interaction.
Another breakthrough is single-sensor technology, which simplifies monitoring by using one optical sensor to measure multiple vital signs, including heart rate, oxygen saturation, temperature, blood pressure, and respiratory rate. A 2026 study in Scientific Reports found this prototype achieved 98.74% accuracy for SpO₂ and 95.47% for heart rate, paving the way for more streamlined, user-friendly devices.
Emerging technologies like Explainable AI (XAI) are also gaining traction. XAI provides clinicians with clear, easy-to-understand insights, which is crucial for building trust in automated systems [14, 17]. Meanwhile, Liquid Neural Networks (LNNs) are being developed to adapt dynamically to real-time data. These networks are particularly effective for tracking rapid physiological changes, such as fluctuating glucose levels in diabetic patients. Together, these innovations promise not only better device performance but also economic benefits for healthcare systems.
Impact on Patient Outcomes and Healthcare Costs
The financial impact of AI-driven monitoring is hard to ignore. With the global elderly population projected to hit 1.5 billion by 2050 and diabetes cases expected to rise from 800 million to 1.3 billion, healthcare systems are under immense pressure to manage costs [1, 3]. By enabling early detection and reducing hospital visits, AI wearables can help mitigate these challenges.
Predictive models using wearable data are already showing remarkable accuracy, with AUC values between 0.92 and 0.94 for conditions like Type 2 Diabetes, COPD, and heart attacks. In chronic kidney disease, these devices have achieved diagnostic accuracies exceeding 99%. This level of precision not only improves patient outcomes but also significantly reduces healthcare costs.
The growing market for wearable healthcare technology highlights its importance. By 2032, the market is expected to surpass $491.74 billion. As these devices become more accessible and reliable, they will support "hospital-at-home" models, easing the burden on traditional healthcare facilities while offering precise monitoring for conditions like heart failure, hypertension, and diabetes.
For products like aiSpine and aiRing, these advancements point to exciting possibilities. Future versions could feature integrated Edge AI, multimodal data analysis, and even smarter predictive algorithms, all while maintaining user-friendly designs that make continuous health monitoring a seamless part of daily life.
Conclusion
AI-powered wearables are reshaping healthcare by moving the focus from treating illnesses after they appear to actively preventing them. Devices like heart rate monitors, temperature sensors, and glucose trackers continuously collect data, which predictive algorithms analyze to identify potential health risks early. This gives healthcare providers the opportunity to step in before conditions worsen, rather than reacting after symptoms develop.
The impact on patient outcomes is clear. A 2025 study by Northwell Health highlighted AI’s ability to predict critical events and ICU transfers well in advance. For chronic conditions such as diabetes – where global cases are projected to rise from 800 million to 1.3 billion by 2050 – these technologies allow for real-time treatment adjustments. This helps reduce complications while easing the strain on patients and healthcare systems alike.
The financial benefits are equally impressive. Wearable biosensors save around $2,840 per patient each year by identifying issues early and cutting down on hospital admissions. When paired with telehealth platforms, these devices have also led to a 43% drop in emergency department visits for monitored patients. These results highlight how AI-driven tools are improving efficiency across healthcare systems.
AIH LLC’s aiSpine and aiRing are prime examples of this trend, offering continuous, personalized monitoring. With advancements in Edge AI, multimodal data fusion, and adaptive algorithms, these devices are set to play an even bigger role in managing spine health, chronic diseases, and overall wellness. They make hospital-grade monitoring an everyday convenience, bringing healthcare closer to where people live.
FAQs
How accurate are AI symptom alerts from wearables?
AI-powered wearables can alert users to potential viral symptoms with around 82% accuracy. They have an impressive ability to correctly identify individuals who are unlikely to develop symptoms, achieving a 97% success rate. However, when using stricter warning thresholds, these devices predict symptom development in only about 34% of cases.
Will my wearable data be shared with my doctor automatically?
AI-powered wearables can automatically share your health data with your doctor. These devices combine biometric tracking with clinical monitoring, allowing for early detection of potential health issues and providing predictive alerts to help improve overall health management.
How do wearables reduce false alarms from exercise or stress?
Wearable devices leverage AI-driven predictive analytics to spot subtle physiological patterns. This allows them to distinguish between typical responses to activity or stress and genuine health issues. The result? Fewer false alarms and more accurate alerts, boosting their overall dependability.