Wearable sensors are changing how chronic diseases like diabetes, cardiovascular issues, and COPD are managed. These devices continuously monitor biomarkers like glucose, blood pressure, and oxygen levels, providing real-time data that helps detect early signs of illness, track disease progression, and personalize treatments. Here’s a quick overview of how they work:
- What They Do: Wearable sensors collect physiological and biochemical data (heart rate, glucose, etc.) through non-invasive methods like sweat, saliva, or skin contact.
- How They Work: They use technologies like electrochemical and optical sensors, flexible electronics, and AI to convert biological signals into actionable health insights.
- Why They Matter: Continuous tracking helps identify health changes early, enabling proactive care and reducing healthcare costs.
Devices like AIH LLC‘s aiSpine (for spine health) and aiRing (for vital signs) integrate with the AIH Health App, offering accessible tools for chronic disease management. These tools highlight how wearable sensors are making healthcare more personalized and effective.
Healthcare IoT: Wearables & Remote Patient Monitoring Explained | Internet of Things
Technologies That Power Wearable Sensors
Wearable sensors rely on a combination of technologies to monitor chronic diseases effectively. These devices integrate three key components: sensing mechanisms to detect biological signals, flexible materials for consistent skin contact, and AI algorithms to process raw data into meaningful health insights. Together, these elements enable continuous and precise health tracking. Let’s break down the core technologies – sensing, microfluidics, and AI – that make this possible.
Electrochemical and Optical Sensing
Electrochemical sensors translate biochemical reactions, such as enzyme activity, into electrical signals like voltage or current. For example, amperometric sensors measure glucose by converting redox reactions into proportional electrical currents. Meanwhile, potentiometric sensors track electrolytes (e.g., sodium, potassium, calcium) in sweat or saliva by detecting voltage differences between electrodes. Cutting-edge designs like electrolyte-gated graphene field-effect transistors have achieved incredible sensitivity, detecting glucose levels as low as 100 attomolars (aM) in tears.
Optical sensors, on the other hand, use light to identify biomolecules through absorption, fluorescence, or scattering. A common example is photoplethysmography (PPG), which tracks heart rate and heart rate variability by measuring blood volume changes under the skin. For more complex tasks, such as detecting trace amounts of drugs or metabolites in sweat, Surface-Enhanced Raman Scattering (SERS) employs nanoengineered metal structures to amplify signals by a factor of 10^11, making it sensitive enough to identify individual molecules.
"The fusion of nanotechnologies with wearable bioelectronics has catalyzed a paradigm shift toward proactive and personalized healthcare, with the potential to drastically improve chronic disease management." – Jiaobing Tu, Andrew and Peggy Cherng Department of Medical Engineering, California Institute of Technology
Microfluidics and Flexible Electronics
Microfluidic systems address the challenge of collecting and transporting small volumes of biofluids like sweat, saliva, or tears to sensor surfaces. They operate without external power, relying on capillary forces, material properties, and hydrophobic valves to manage fluid flow and activate reagents. Innovative designs inspired by tree branches can increase biofluid collection rates by 10–100 times, while advanced systems refresh sweat samples in roughly one minute, ensuring real-time monitoring rather than outdated readings.
Flexible electronics resolve the mismatch between rigid sensors and the human body’s dynamic movements. Materials like PDMS, polyimide, and hydrogels allow sensors to bend and stretch, maintaining reliable skin contact and reducing noise caused by motion. These flexible electrodes can endure up to 10,000 bending cycles while retaining functionality. Additionally, encapsulation techniques like photo-patternable Ecoflex improve performance under strain, achieving 50% higher conductance at 250% elongation compared to traditional materials. The result? Lightweight, breathable devices that minimize irritation during extended use, with some achieving heart rate accuracy within ±6 bpm and temperature monitoring with a minimal standard deviation of 0.14%.
AI Integration for Data Analysis
Hardware alone isn’t enough – AI steps in to turn raw data into actionable insights. Artificial intelligence processes the constant stream of physiological data from wearable sensors, filtering out noise, identifying patterns, and predicting health events before symptoms arise. A 2025 review emphasized AI’s role in enabling continuous monitoring for early disease detection and managing chronic conditions like diabetes and heart disease, addressing the growing global health challenges. Another study from the same year demonstrated how AI algorithms could analyze multimodal data from wearable sensors, identifying acute events like cardiac arrhythmias in under a second and significantly improving patient outcomes.
"The integration of artificial intelligence with wearable bioelectronics is revolutionizing digital healthcare by enabling proactive, personalized, and data-driven medical solutions." – Guangqi Huang, Author, MDPI
How Wearable Sensors Work: Step-by-Step Process
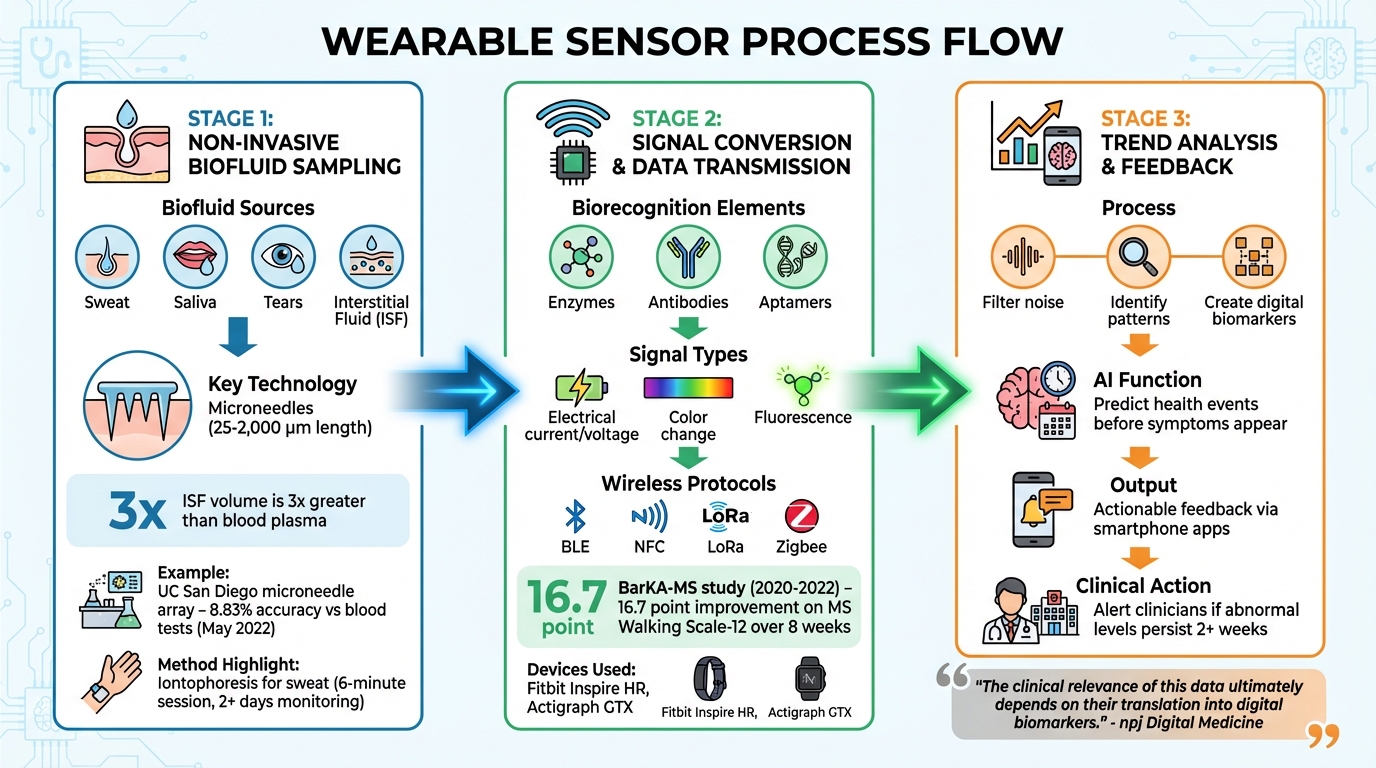
How Wearable Sensors Convert Biological Signals Into Health Data
Wearable sensors turn biological signals into useful health data through three main stages: sampling, signal conversion, and trend analysis.
Non-Invasive Biofluid Sampling
Wearable sensors rely on biofluids like sweat, saliva, tears, and interstitial fluid (ISF) to access biomarkers. ISF, the fluid surrounding cells just beneath the skin, is particularly valuable since it exists in volumes nearly three times greater than blood plasma in the body.
Microneedle technology offers a minimally invasive way to access ISF. These tiny needles, measuring between 25 and 2,000 μm (0.001 to 0.08 inches), penetrate only the outer skin layer to reach the dermis where ISF is found. Because they avoid nerve endings and blood vessels, the process is painless. In May 2022, researchers at the University of California San Diego tested a wearable microneedle array that wirelessly sent real-time glucose and alcohol data to a smartphone app. The results showed a mean absolute relative difference of 8.83% compared to standard blood tests.
Sweat-based monitoring uses iontophoresis, which induces sweat with a mild electrical current. In August 2025, Wei Gao’s team at Caltech introduced the BMS3, a sweat sensor inspired by biology. This device tracked uric acid, xanthine, and alcohol levels for over two days after a single 6-minute iontophoresis session in clinical tests.
Other designs incorporate sensors into everyday items like mouthguards (for saliva), contact lenses (for tears), and even face masks that capture biomarkers from exhaled breath.
"Microneedle (MN) technology provides a solution for the wearable technologies to sample biofluid, detect biomarkers, and monitor electrophysiological signals." – Tianli Hu et al., City University of Hong Kong
Once biofluids are collected, the next step is converting biomarkers into usable data.
Signal Conversion and Data Transmission
After sampling, biorecognition elements such as enzymes, antibodies, or aptamers bind to specific biomarkers. This interaction generates a measurable signal – commonly an electrical current or voltage for electrochemical sensors, or a color change or fluorescence for optical sensors.
Wearable devices then translate these signals into digital data using onboard electronics. This data is transmitted wirelessly to smartphones or cloud platforms using low-power protocols like BLE (Bluetooth Low Energy), NFC, LoRa, or Zigbee.
For example, the BarKA-MS study (2020–2022) showed how sensor data from devices like Fitbit Inspire HR and Actigraph GTX, combined with self-reported surveys, helped create digital biomarkers. Over an 8-week period, these biomarkers correlated with improvements of 16.7 points on the MS Walking Scale-12.
Once the data is transmitted, it undergoes analysis to identify patterns and trends.
Trend Analysis and Feedback
Raw data is processed to filter out irrelevant information, like weather effects or unrelated activities, and to highlight meaningful patterns. This process creates digital biomarkers.
Using AI, wearable systems analyze continuous streams of physiological data to predict potential health events before symptoms appear. For instance, AI can differentiate between heart rate spikes caused by exercise and those signaling cardiac arrhythmias, ensuring alerts are issued only for clinically significant events.
Finally, users receive actionable feedback via smartphone apps. These insights help them understand physiological changes in real time. In clinical settings, digital biomarkers can trigger specific actions, such as notifying a clinician if glucose levels remain abnormal for two consecutive weeks.
"The clinical relevance of this data ultimately depends on their translation into digital biomarkers." – npj Digital Medicine
sbb-itb-44aa802
AIH LLC Devices for Biomarker Tracking
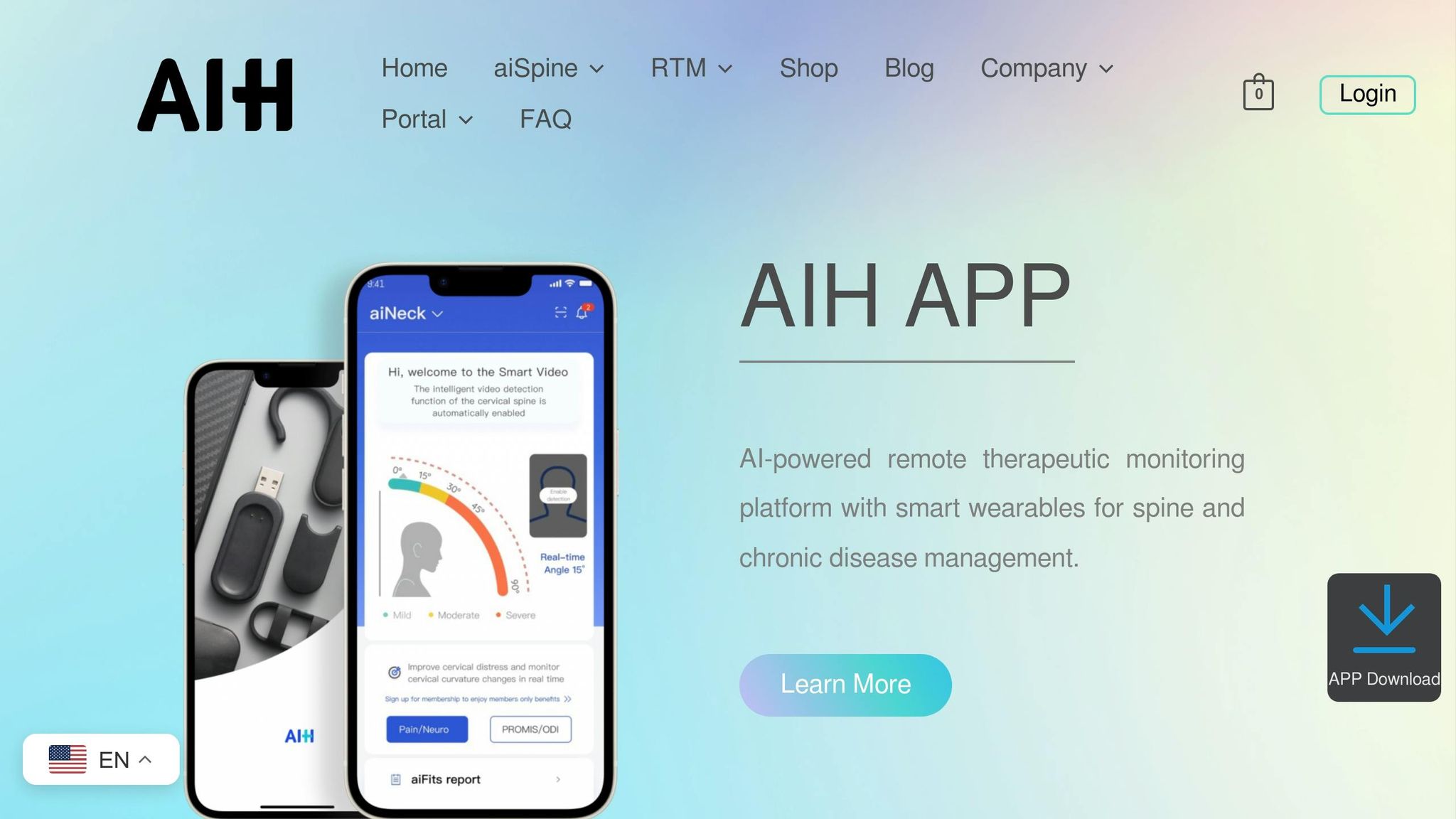
AIH LLC has developed advanced tools that combine sensing technologies with innovative design to support continuous monitoring of chronic conditions. Two standout devices in their lineup are aiSpine, focused on spine health, and aiRing, designed for tracking vital signs. Both devices integrate seamlessly with the AIH Health App, providing real-time biomarker data and tailored health insights.
aiSpine: Monitoring Spine Health

The aiSpine device incorporates a 9-axis IMU sensor to track spinal alignment and posture-related biomarkers, including activity levels and calories burned. This compact device offers multiple wear options – ear, glasses, or clip-on – making it adaptable for targeted spine monitoring. It connects via Bluetooth 4.0 and features a 7-day standby battery life.
Using aiSpine is straightforward, thanks to a simple three-step calibration process:
- Position the device.
- Maintain a natural posture while selecting "Start Calibration."
- Bend the neck for two seconds until a short vibration confirms setup.
Once calibrated, the device alerts users to poor posture through haptic feedback and sends notifications to the AIH Health App. At a discounted price of $49.00 (originally $99.00), aiSpine offers an accessible solution for managing chronic back and neck pain through continuous posture correction.
While aiSpine focuses on spinal health, AIH LLC’s aiRing expands monitoring to broader physiological metrics.
aiRing: Real-Time Vital Sign Tracking
The aiRing device uses a combination of precision sensors and AI to monitor vital signs continuously. Unlike aiSpine, which targets biomechanical markers, aiRing captures physiological data to support overall health.
"aiRing is an artificial intelligence (AI) driven device equipped with ultra-low power Bluetooth chips and various precision sensors, integrating autonomous AI algorithms to intelligently obtain physical health data." – AIH LLC
With a waterproof design and intelligent touch controls, aiRing is perfect for activities like sleep tracking and exercise monitoring. Data streams directly to the AIH Health App for real-time analysis. The device is available in two models:
- aiRing Ultra: $57.00 (reduced from $169.00)
- aiRing Lite: $49.90 (reduced from $69.00)
Integration with the AIH Health App
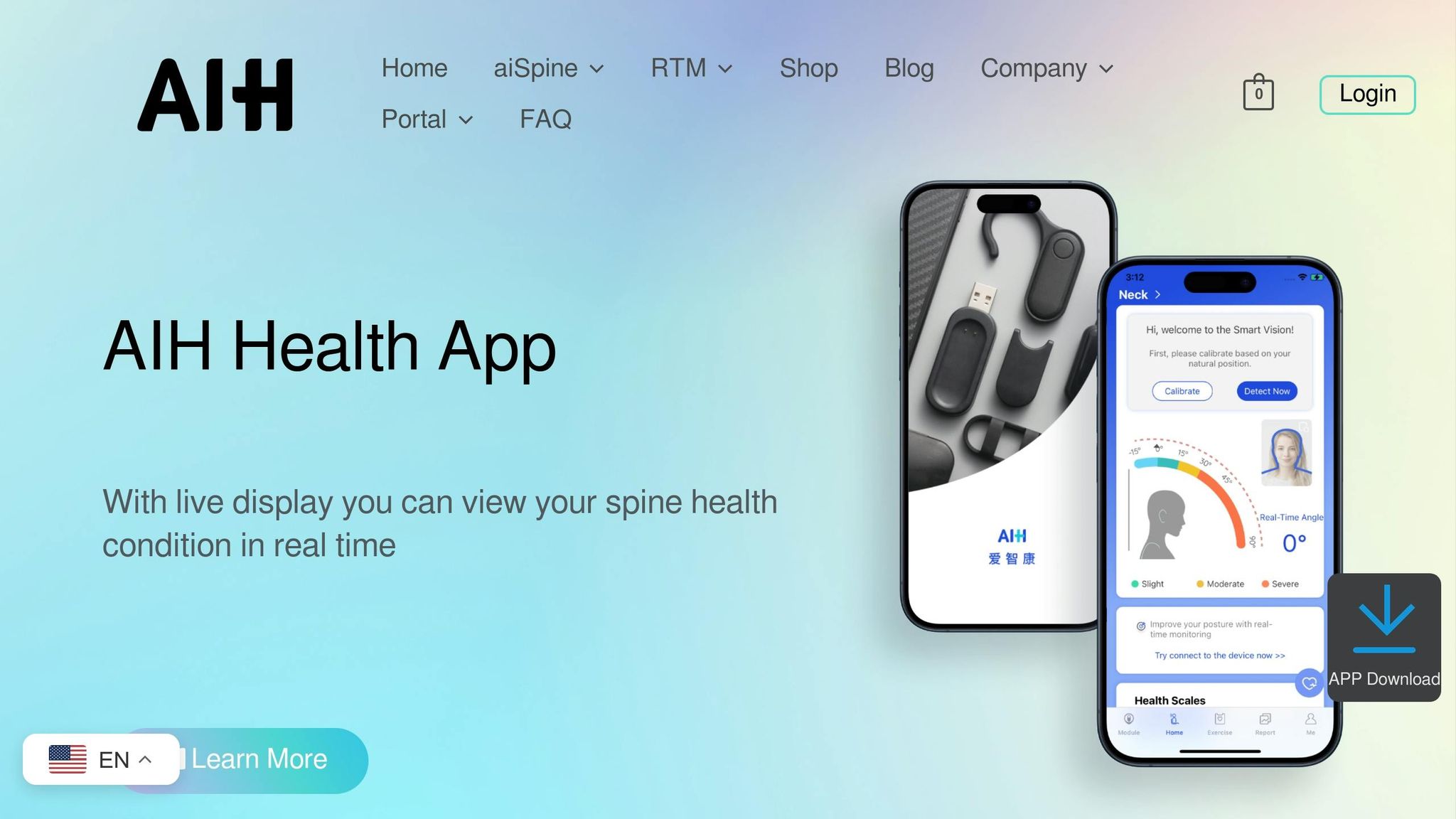
Both aiSpine and aiRing sync with the AIH Health App, creating a centralized hub for biomarker tracking and personalized care. The app’s "Live Display" feature provides real-time updates on spine health, including cervical and lumbar alignment changes.
"With live display technology, you can view your spine health condition in real time directly on the AIH Health App." – AIH LLC
Beyond real-time monitoring, the app analyzes historical data to identify trends and develop personalized health models based on users’ sitting and standing patterns. For chronic disease management, the platform supports Remote Therapeutic Monitoring (RTM), enabling healthcare providers to oversee musculoskeletal and respiratory conditions, track therapy adherence, and assess treatment outcomes.
AIH Health App also prioritizes data security, ensuring that health information is accessible only to users and authorized medical professionals. Looking ahead, the platform will integrate data from upcoming devices like aiBP (blood pressure monitoring) and aiGlucoCare (glucose tracking), creating a comprehensive system for managing chronic conditions.
Conclusion
Wearable sensors are reshaping how chronic diseases are managed by leveraging cutting-edge technology and a systematic approach. Combining electrochemical sensing, flexible electronics, and AI-driven data analysis, these devices monitor biomarkers continuously, often detecting health changes before symptoms even appear.
"The synergy between AI and wearable bioelectronics is shifting this paradigm toward proactive, personalized, and data-driven solutions." – MDPI
The stakes are high: chronic diseases are responsible for 41 million deaths annually. With the global population aged 60 and older expected to double by 2050, scalable and efficient health monitoring becomes more critical than ever. Key advancements, like AI algorithms that filter out data noise and edge computing that reduces latency to under 20 milliseconds, are making real-time, individualized health tracking a reality. By focusing on personal health trends rather than generic averages, these technologies pave the way for precise detection and targeted care.
AIH LLC offers a glimpse into this future with its innovative devices. The aiSpine tracks spinal health through posture monitoring, while the aiRing provides discreet, continuous vital sign tracking. Both seamlessly integrate with the AIH Health App, which supports Remote Therapeutic Monitoring and creates personalized health models based on an individual’s unique baseline. These tools highlight how continuous monitoring is revolutionizing chronic disease management.
Wearable sensors are empowering patients and healthcare providers alike, moving healthcare from sporadic clinic visits to continuous, data-informed care. This shift not only extends lives but also enhances their quality.
"You can’t manage what you can’t measure." – Peter Drucker
FAQs
How accurate are wearable biomarker readings versus lab tests?
Wearable devices for biomarker readings have made strides in accuracy, though they still fall short of the precision offered by lab tests. Thanks to advancements in nanotechnology and biomolecular sensing, these devices are becoming more dependable for real-time monitoring. However, challenges like device calibration and differences between individuals can impact their precision. While wearables are excellent for providing continuous data, especially for managing chronic conditions, they often need to be cross-checked with lab tests to confirm their accuracy – particularly when it comes to critical diagnostic decisions.
How does AI tell a real health issue from normal activity noise?
AI leverages sophisticated machine learning algorithms, trained on vast datasets, to differentiate real health concerns from everyday activity noise. These systems identify patterns associated with health issues, such as irregular heartbeats, while ignoring harmless signals caused by movement or external factors. By detecting subtle changes in sensor data, AI minimizes false alarms, providing accurate alerts that support early intervention and help manage chronic conditions effectively.
Are wearable sensor health data private and secure?
Wearable sensors collect highly sensitive health data, making privacy and security a top priority. Safeguarding this information often relies on tools like encryption, secure storage systems, and strict access controls to prevent unauthorized access. As AI and machine learning become more integrated into wearable technology, protecting user data isn’t just a technical challenge – it’s essential for maintaining trust and adhering to privacy regulations. Efforts to improve these protections continue to evolve alongside technological advancements.