AI is transforming healthcare by making wearable device data useful for Electronic Health Records (EHRs). Wearables like smartwatches and fitness trackers collect continuous health data such as heart rate, sleep patterns, and glucose levels. However, EHRs are designed for clinic-based, episodic data, creating a gap. AI bridges this gap by cleaning, standardizing, and summarizing wearable data so it fits seamlessly into EHR systems. The result? Doctors get a clearer, more complete view of a patient’s health, enabling earlier interventions and better chronic disease management.
Key Takeaways:
- AI refines wearable data: It removes noise, fills gaps, and aligns data with medical standards (e.g., FHIR).
- Improved predictions: Combining wearable data with EHR improves health outcome predictions by up to 12.6% for diabetes and 9.7% for hypertension.
- Privacy-focused solutions: Federated learning ensures data security by processing information locally on devices.
- Easier clinician workflows: AI integrates wearable data directly into EHRs, reducing manual work and improving decision-making.
This integration is already reducing hospitalizations, improving treatment adherence, and saving healthcare providers time and money.
MyVitals: Connecting Wearable Health Data to EHRs with InterSystems
AI Technologies That Enable Wearable-EHR Integration
AI is the bridge that connects continuous data from wearable devices to the episodic records stored in EHR systems, turning raw information into actionable clinical insights. Middleware powered by AI plays a critical role in converting wearable data into formats that align with EHR standards. For instance, deep learning models can analyze physiological signals like ECG or heart rate variability, filtering out noise and identifying key patterns that matter clinically. Transformer models, in particular, have demonstrated impressive capabilities, achieving 96.1% classification accuracy with just 30ms latency. This makes real-time health monitoring not only possible but practical.
Another standout technology is federated learning, which trains models locally on devices rather than transferring sensitive data to centralized servers. This approach not only protects privacy but also achieves a 98.9% success rate in detecting tampering, reducing privacy risks by 90%. Meanwhile, generative AI steps in to fill data gaps, ensuring that analysis remains reliable even when patients forget to wear their devices or if data transmission fails. Together, these technologies create a foundation for standardized, actionable data that fuels predictive analytics.
AI for Data Standardization and Interoperability
AI simplifies the process of converting raw wearable data into formats that work seamlessly with EHR systems. It maps these readings to FHIR (Fast Healthcare Interoperability Resources) standards, creating structured resources like Observation, Device, and Patient that are universally readable by any compliant EHR platform. For example, a heart rate measurement from a wearable device is translated into the LOINC code 8867-4, while SpO2 readings are mapped to 59408-5. This ensures that data from devices like aiRing is interpreted the same way across platforms like Epic or Oracle Health.
AI preprocessors also bridge the gap between modern and legacy systems by mapping wearable data to FHIR standards while converting older HL7 messages. Deep learning further enhances data quality by filtering out motion artifacts and outliers that could otherwise lead to false alerts.
Predictive Analytics for Clinical Decision Support
After harmonizing the data, AI shifts its focus to proactive risk assessment. Instead of using generic thresholds, machine learning models establish a personalized physiological baseline for each patient. These models can detect deviations from the norm, flagging potential health issues 48–72 hours before clinical deterioration occurs. This tailored approach is essential because what’s "normal" for one patient may signal a problem for another.
Large Language Models (LLMs) add another layer of sophistication by synthesizing months of wearable data alongside episodic EHR records. They produce concise summaries that help clinicians identify trends without the need to sift through endless spreadsheets.
"Good alerting should feel quiet most of the time. The point is one clear next step with a short explanation that a human can verify in seconds."
– Slava Khristich, CTO at TATEEDA GLOBAL
How to Implement AI-Driven Wearable-EHR Integration
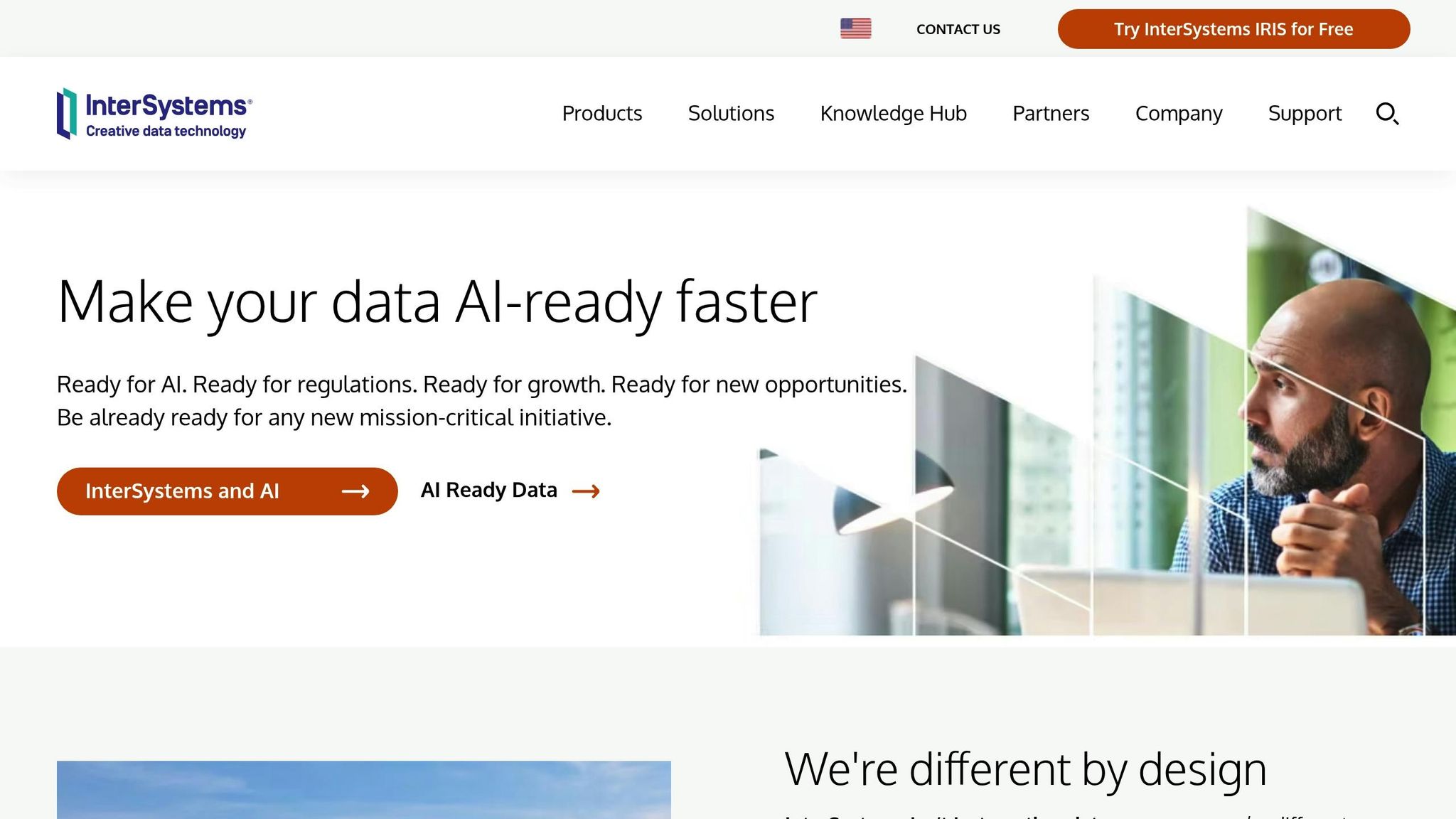
5-Step AI-Driven Wearable-EHR Integration Implementation Process
Integrating wearable devices with Electronic Health Records (EHRs) requires a structured approach to ensure security, data quality, and clinical relevance. This process transforms raw sensor data into actionable insights that fit seamlessly into a clinician’s workflow. Organizations can choose from three main integration paths: Path A (direct device cloud to EHR via API), Path B (using data aggregators to unify diverse device APIs), or Path C (building a custom HIPAA-compliant pipeline for full control). With remote patient monitoring claim volumes in the U.S. surging by about 1,294% between 2019 and 2022, and one in three U.S. adults using health wearables – over 80% of whom are open to sharing their data with clinicians – there’s a clear opportunity to streamline this process. The challenge lies in converting this data-sharing willingness into a secure, standardized flow. Below are the steps to securely collect, process, analyze, transfer, and protect wearable data.
Step 1: Collect Wearable Data via Secure APIs
The starting point is data collection, which relies on OAuth 2.0 authentication to secure access to wearable platforms. Developers must register their applications with providers like Apple HealthKit, Fitbit, or Google Fit, specifying the data they need (e.g., heart rate, SpO₂, or sleep stages) through a user consent flow. This generates access tokens for retrieving time-stamped physiological data and refresh tokens for uninterrupted data collection.
For devices such as aiSpine and aiRing, secure APIs are used to pull posture metrics and vital signs from the AIH Health App. Authorization codes are exchanged for tokens, which are stored in encrypted vaults to prevent unauthorized access. A 2025 study highlighted the effectiveness of collecting wearable data via secure APIs and mapping it to HL7 FHIR resources.
Step 2: Process and Clean Data with AI Middleware
Once data is collected, AI middleware takes over to clean and standardize it. This involves removing noise, validating accuracy, and ensuring consistency. Using a "sidecar" pattern, AI components integrate with legacy EHR systems without disrupting their stability. Signal-processing algorithms clean single-lead ECG data and correct motion artifacts in SpO₂ and respiration readings. Biological plausibility checks flag anomalies – like heart rates outside the 30–250 bpm range – while duplicate submissions are filtered out. The middleware then converts this heterogeneous data into standardized HL7 FHIR resources, aligning timestamps and units for smooth trend analysis before committing the data to the clinical record.
Step 3: Analyze Data and Generate Alerts with AI
After processing, AI tools analyze the data in real time, creating personalized physiological baselines for each patient. Alerts are triggered only when patients deviate from their normal patterns, cutting down on unnecessary notifications. Research shows AI-powered alert systems can reduce false alarms by 35% compared to traditional methods.
For instance, aiSpine users benefit from AI that monitors posture patterns, detecting prolonged slouching or abnormal spinal alignment and prompting timely interventions. Similarly, aiRing tracks vital signs continuously, flagging potential health concerns 48–72 hours before clinical deterioration. A real-world example: between 2025 and 2026, the Mayo Clinic implemented a system where AI analyzed Apple Watch ECGs to detect asymptomatic left-ventricular dysfunction, enabling clinicians to review processed trends directly in the EHR.
Step 4: Transfer Data to EHR Systems
The next step is transferring analyzed data into the EHR as structured FHIR resources. Middleware ensures idempotent writes using request keys, avoiding duplicate records. Data is mapped to specific FHIR endpoints like Observation (vitals), Device (hardware identifiers), and Patient (demographics). This allows clinicians to view wearable data trends directly within their EHR workflow. Additionally, the integration supports automated data capture for remote patient monitoring billing codes, including CPT 99453 (setup), 99454 (data transmission), and 99457/99458 (clinical review).
Step 5: Maintain HIPAA Compliance and Data Security
Throughout the entire process, maintaining HIPAA compliance and data security is essential. This includes establishing Business Associate Agreements, applying redaction and de-identification techniques to protect PHI, and using OAuth 2.0 or OpenID Connect for secure identity management with least-privilege access scopes. Encrypted token vaults safeguard API credentials, while tamper-evident audit logs stored in immutable write-once, read-many systems support compliance audits. Federated security frameworks for wearables can detect tampering with a 98.9% success rate, and federated learning approaches reduce privacy risks by up to 90%. Data in transit is protected with TLS, and data at rest is encrypted using AES-256.
Benefits of AI-Powered Wearable-EHR Integration
The integration of AI-powered systems with wearable devices and electronic health records (EHRs) is reshaping how chronic diseases are managed. By blending continuous data from wearables with clinical records, this approach allows for proactive care and tailored interventions. Instead of relying on fragmented, episodic health records, clinicians can now access a comprehensive view of a patient’s health, combining medical history with daily behavioral patterns. This shift improves the accuracy of predictions across a variety of clinical outcomes.
The results of proactive care speak for themselves. AI-enabled wearables have contributed to a 25% reduction in hospitalization rates for chronic diseases. For instance, the CHAMPION study found that integrating hemodynamic monitoring for heart failure patients reduced hospital admissions by 28% over 18 months. In diabetes management, AI-driven glucose prediction models have achieved over 85% accuracy within a 1–2-hour timeframe, with 60% of studies reporting error rates under 15 mg/dL – well within acceptable clinical standards. Moreover, treatment adherence has increased by 30% when patients receive real-time, personalized feedback from AI-powered systems.
Healthcare providers are also seeing tangible benefits. For example, ExpressMED, an occupational medicine provider in New Hampshire, integrated wearable data with the PrognoCIS EHR system in July 2025. This integration eliminated manual data entry, saving about 10 hours per week per location. Similarly, BloodLnk achieved a 20% reduction in operational costs and saved 24 staff hours weekly through automated data handling. Athens Neurology reported annual savings of over $82,000 after adopting an AI-integrated EHR system, which also boosted practice efficiency.
"Connecting physical activity data directly into EHR workflows gives clinicians a more complete picture of a patient’s health, enhancing patient conversations and behavior change recommendations." – Drew Schiller, CEO, Validic
Devices like aiSpine and aiRing exemplify how this streamlined integration supports proactive health management. These tools allow clinicians to monitor posture patterns and vital signs continuously within their existing EHR workflows. By consolidating data monitoring into a single system, clinicians can intervene before a patient’s condition worsens, ensuring timely and effective care.
Pre-AI vs. AI-Powered Integration: A Comparison
The table below highlights the clear advantages of AI-powered workflows over traditional methods:
| Metric | Traditional (Pre-AI) Integration | AI-Powered Integration |
|---|---|---|
| Data Monitoring | Intermittent/static (clinic visits only) | Continuous/real-time tracking |
| Data Accuracy | Prone to manual entry errors and device noise | AI filters noise and fills in missing data |
| Alert Response Time | Reactive; alerts triggered after events occur | Proactive; predicts events hours in advance |
| Chronic Disease Effectiveness | Fragmented data silos; episodic review | Holistic predictions combining lifestyle and clinical data |
| Workflow Efficiency | Manual uploads; switching between dashboards | Automated sync with EHR workflows |
| Patient Adherence | Lower; relies on self-motivation | 30% higher; driven by real-time feedback |
| Provider Workload | High; manual data interpretation required | Reduced; automated processing and detection |
sbb-itb-44aa802
Case Study: Integrating aiSpine and aiRing with EHR Platforms
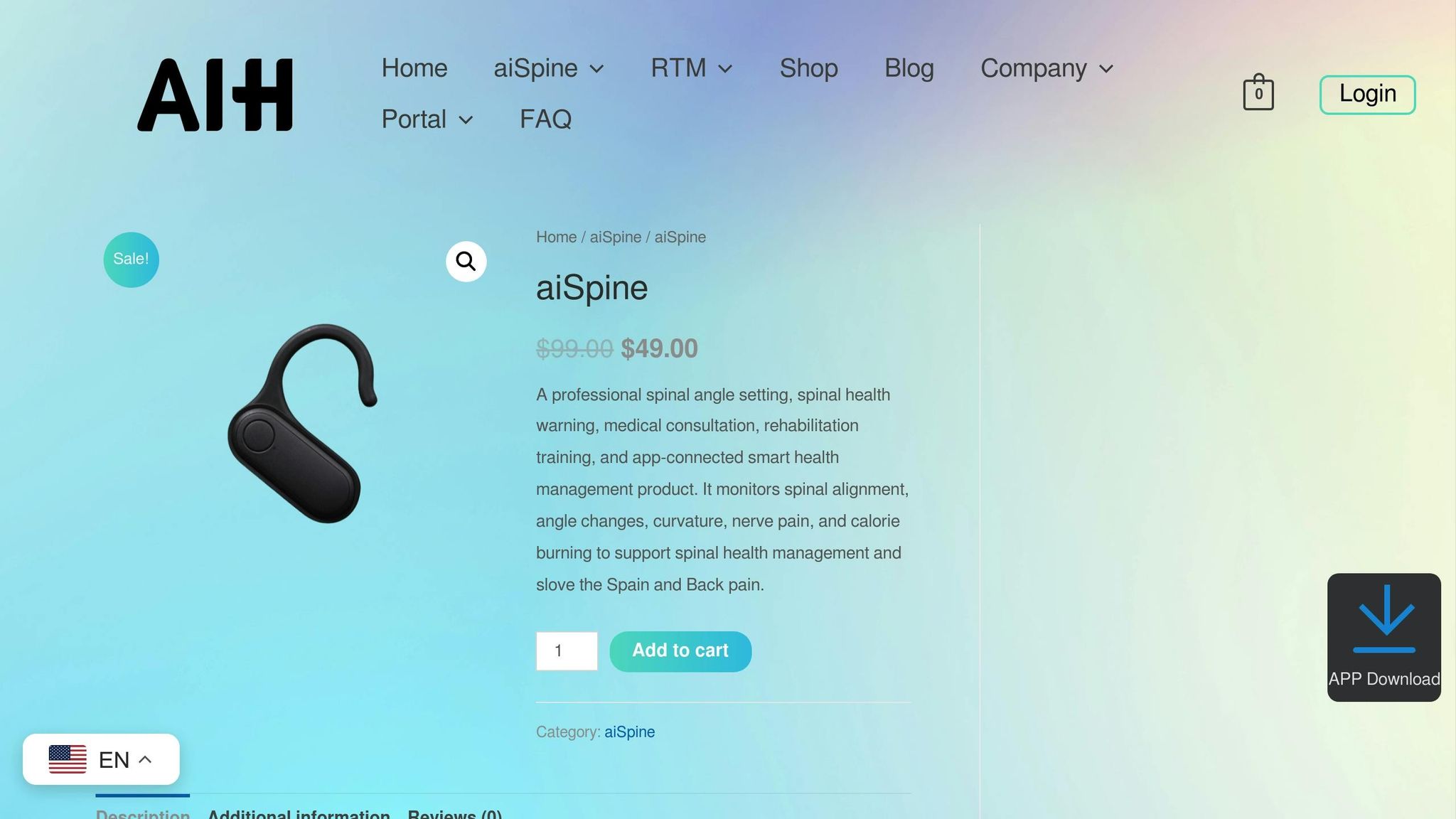
AIH LLC‘s aiSpine and aiRing devices showcase how AI-powered wearables can work smoothly with EHR platforms to provide continuous, actionable health insights. The aiSpine employs MEMS motion sensors to monitor posture, step counts, and activity classification, while the aiRing uses biosensors to track heart rate (HR), heart rate variability (HRV), skin temperature, and SpO2 levels. Both devices transmit their data wirelessly to the AIH Health App using secure protocols. From there, AI middleware processes the raw signals, cleaning and normalizing the data before sending it to the EHR.
The integration process is carefully designed to ensure both clinical accuracy and HIPAA compliance. It starts with the AIH Health App securely pulling authorized data using OAuth 2.0 or OpenID Connect (OIDC) for identity management. AI algorithms then filter out noise and motion artifacts, aligning the data to each patient’s unique baseline rather than relying on generic thresholds. This personalized approach ensures that normal variations, like a heart rate increase during exercise, aren’t flagged as issues, while subtle changes that might signal early health concerns are detected.
After the data is cleaned, it is converted into HL7 FHIR resources using standardized LOINC codes. For instance, heart rate data from the aiRing is mapped to the FHIR Observation code 8867-4, and aiSpine’s posture metrics are categorized for musculoskeletal health tracking. This standardization ensures compatibility across various EHR systems. Before the data is uploaded, validation layers check for errors, such as heart rates outside the 30–250 bpm range, and prevent duplicate entries.
The AIH Health App integrates this processed data into clinician workflows through a SMART on FHIR interface. Instead of overwhelming providers with raw data, the system embeds trendlines and AI-generated summaries directly into the EHR environment. Clinicians receive concise, actionable insights – like a risk score for deterioration or a weekly summary of posture trends – enabling quicker and more informed decisions. Slava K., CEO of TATEEDA, explains: "Good alerting should feel quiet most of the time. The point is one clear next step with a short explanation that a human can verify in seconds".
For patients, the AIH Health App simplifies complex physiological data into easy-to-understand guidance. It provides real-time feedback on posture correction and trends in vital signs, encouraging better adherence to treatment plans. Throughout the entire process, the pipeline adheres to strict HIPAA requirements with Business Associate Agreements (BAAs), end-to-end encryption (TLS), PHI segregation, and tamper-evident audit logs ensuring compliance.
Technical Components for AI Wearable-EHR Pipelines
This section dives into the essential technical elements that turn raw data from wearable devices into meaningful clinical insights. A well-designed AI-powered wearable-EHR pipeline securely gathers data, processes it, and delivers actionable outcomes, all while adhering to HIPAA standards and meeting clinical needs.
The system architecture often employs a sidecar model, where AI functionality operates alongside the EHR system rather than altering its core. This setup keeps the EHR stable while allowing AI models to evolve as new algorithms are developed. With the growing demand for remote patient monitoring, these pipelines must also be scalable and efficient.
A standout feature of modern pipelines is federated learning, which trains AI models directly on devices. This method not only enhances privacy but also strengthens tamper detection. Additionally, reinforcement learning-based adaptive sampling can reduce wearable device power usage by 50%, extending battery life without compromising data quality. These design choices pave the way for advanced AI tools that streamline data integration and processing.
AI Components and Their Functions
Here’s a breakdown of the core AI components and their roles in the pipeline:
| Component | Purpose | Key AI Features |
|---|---|---|
| Ingest API | Pulls authorized data from device clouds (e.g., Apple HealthKit, Fitbit, Garmin) | Automated token refresh logic, OAuth 2.0/OIDC consent handling, secure token vault management |
| AI Transformer | Normalizes units, cleans noise, and aligns data streams | Deep learning for signal denoising (e.g., ECG/EEG), automates LOINC mapping, corrects clock drift, filters motion artifacts |
| Prediction Models | Analyzes trends and flags clinical risks | Anomaly detection based on patient-specific baselines, 48–72 hour risk scoring, human-readable summary generation |
| FHIR Writer | Transfers processed data to EHR systems | Automated resource bundling into HL7 FHIR format, idempotent write-back logic to avoid duplicates |
| SMART on FHIR App | Integrates insights into clinician workflows | Natural language summaries, confidence score visualization, trendline displays |
The AI Transformer excels with a 96.1% classification accuracy on physiological signals, achieving this with just a 30 ms processing latency, enabling real-time data handling. Meanwhile, the FHIR Writer employs idempotent write-back logic, ensuring that network retries don’t create duplicate entries in patient records. Together, these components create a seamless system that transforms raw sensor data into reliable, actionable clinical insights.
Conclusion
AI-powered integration of wearable devices with Electronic Health Records (EHR) is reshaping how chronic diseases are managed. By combining data from wearables, EHR systems, and patient-reported outcomes, AI provides a comprehensive, long-term view of a patient’s health that was previously unattainable. This shift takes healthcare from a reactive, symptom-focused approach to one that is proactive and predictive, addressing potential issues before they escalate into serious conditions.
For example, AI models enhanced with wearable data have shown measurable improvements in predicting chronic conditions, with a 12.6% boost in AUROC for diabetes and 9.7% for hypertension. Deepa Fernandes Prabhu from the Center for Decision Support Systems and Informatics highlights this shift:
"The integration of Artificial Intelligence, Electronic Health Records (EHRs), and wearable technologies holds substantial potential for transforming healthcare from a reactive, disease-focused model to a proactive, patient-centered paradigm."
Technical frameworks play a critical role in making this integration seamless. Tools like secure APIs, AI middleware, FHIR writers, and SMART on FHIR applications ensure that data is cleaned, standardized, and converted into actionable insights. These systems not only manage the challenge of overwhelming data volumes but also maintain the precision required for clinical decisions. For healthcare providers, adopting interoperability standards such as HL7 FHIR, ensuring AI transparency, and creating user-friendly interfaces are essential for successful implementation. Such efforts pave the way for smoother workflows and better adoption by both patients and clinicians.
Future developments in areas like federated learning and blockchain security are set to build on these successes, driving the Internet of Medical Things (IoMT) market toward an estimated $135.87 billion by 2025. Meanwhile, technologies like liquid neural networks promise enhanced adaptability and privacy in real-time applications. Companies like AIH LLC, with devices such as aiSpine and aiRing, are already leveraging these advancements to provide continuous monitoring and personalized health feedback, improving patient outcomes.
AI is not just improving wearable-EHR integration – it is making it a scalable and practical solution for tackling the increasing challenges of chronic disease management. Healthcare providers who embrace these systems now are poised to deliver superior care, reduce costs, and engage patients more effectively.
FAQs
How does AI protect wearable health data when linking it to EHRs?
AI plays a key role in protecting the privacy and security of data from wearable health devices when integrating it with Electronic Health Records (EHRs). It uses tools like encryption to secure data both while it’s being transmitted and when it’s stored, anonymization to strip away personal identifiers, and strict access controls to block unauthorized access. These practices align with regulations such as HIPAA, ensuring that sensitive health data stays protected.
AI systems are also built to uphold data integrity and transparency, addressing ethical concerns and building trust with users. By using privacy-first frameworks and adhering to strict standards, AI not only safeguards patient information but also enables the seamless and secure connection of wearable device data with EHRs.
How does AI improve the integration of wearable devices with EHRs for managing chronic conditions?
AI is transforming how wearable devices interact with electronic health records (EHRs), making data collection and analysis smoother. This allows for real-time monitoring and tailored care for individuals managing chronic conditions. By leveraging predictive analytics, AI can flag potential health concerns early, giving healthcare providers the tools to make better-informed decisions.
With automated processing, AI ensures that data from wearables – like heart rate, activity levels, or sleep patterns – flows directly into EHRs without the need for manual entry. This creates a fuller picture of a patient’s health, helping doctors craft more effective treatment plans. The outcome? A healthcare approach that’s more efficient and focused on keeping patients healthier.
How does AI improve the accuracy and security of wearable data integration with EHRs?
AI technologies like federated learning and deep learning models are transforming how wearable data integrates with Electronic Health Records (EHRs), boosting both accuracy and security. Federated learning processes data directly on devices, meaning sensitive health information doesn’t need to be sent to central servers. This approach keeps personal health data private and minimizes the risk of breaches.
Deep learning models take it a step further by analyzing the complex data wearables collect, enabling highly accurate health predictions and tailored insights. To strengthen trust and transparency, privacy-focused techniques such as differential privacy and explainability tools are also used. Together, these advancements ensure wearable-EHR integration is safer and more dependable, paving the way for effective remote health monitoring.