Wearable devices are transforming post-surgical care by offering continuous, non-invasive temperature monitoring. Unlike periodic checks, these devices provide real-time data, detecting fever spikes or hypothermia earlier, which can prevent complications like infections or sepsis. For example, the iThermonitor WT705 identified fevers 4.35 hours earlier than mercury thermometers, while the SteadyTemp patch detected fever in 93.9% of cases, compared to 36.4% with infrared thermometers.
Key takeaways:
- Continuous monitoring: Tracks temperature every 1-4 minutes, reducing missed signs of infection.
- Patient comfort: Non-invasive designs avoid the discomfort of traditional probes.
- AI integration: Enhances accuracy by adjusting for external factors and predicting complications before they escalate.
- Clinical impact: Faster detection leads to quicker treatment, fewer ICU readmissions, and shorter hospital stays.
Despite their benefits, challenges like skin contact issues, false alerts, and occasional data gaps remain. However, advancements in AI and wearable technology are paving the way for smarter, more reliable post-surgical monitoring systems.
Acute Care and Wearable Tech pt 3: Technological requirements for wearable monitoring on the floor
sbb-itb-44aa802
Recent Studies on Wearable Devices for Post-Surgery Temperature Monitoring
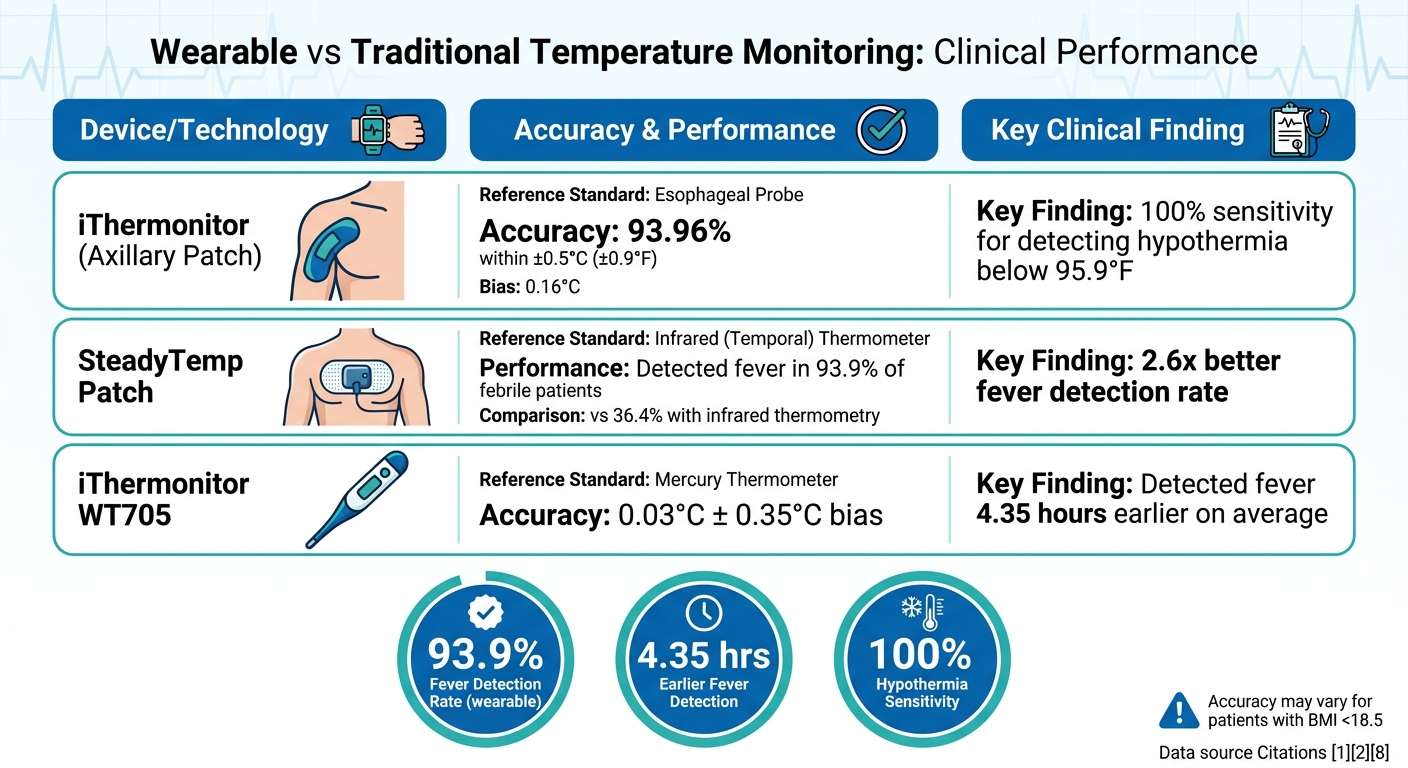
Wearable Temperature Monitors vs Traditional Methods: Performance Comparison
Fiber Bragg Grating (FBG)-Based Wearable Sensors
Fiber Bragg Grating (FBG) sensors offer a novel way to monitor temperature by detecting shifts in light wavelengths as they pass through optical fibers. These shifts correspond to temperature changes, but the sensitivity of bare FBG sensors can be limited.
In May 2024, researchers P. B. Prathap and K. Saara from Dayananda Sagar University and Malnad College of Engineering tackled this issue in a study published in the Journal of Optics. They enhanced FBG sensors by embedding them into a 3D-printed Polylactic Acid (PLA) device. PLA is both biodegradable and biocompatible, making it suitable for medical use. To further boost thermal sensitivity, they added a thin copper layer, leveraging copper’s excellent thermal expansion properties.
Their findings showed that the device could reliably track body temperature changes, providing a non-invasive alternative to traditional methods like esophageal or rectal probes. This approach not only improves patient comfort but also maintains high accuracy in temperature monitoring.
The integration of optical technology with flexible, 3D-printed designs highlights the growing potential of wearable devices for continuous, non-invasive monitoring.
Flexible and 3D-Printed Wearable Systems
At Beijing Tongren Hospital, researchers evaluated the iThermonitor CW106A, a flexible patch designed for precise temperature monitoring. Between December 2023 and May 2024, they tested the device on 80 adult patients undergoing thoracoscopic surgery, comparing 3,536 temperature readings from the patch to those from esophageal probes. The results were impressive: the iThermonitor achieved 93.96% accuracy within a ±0.5°C margin and demonstrated 100% sensitivity in detecting hypothermia below 95.9°F.
"The iThermonitor is a reliable and accurate non-invasive alternative to traditional invasive temperature monitoring methods in thoracoscopic surgery."
– Guyan Wang, Beijing Tongren Hospital
Such accuracy is critical for timely medical intervention, particularly in the delicate post-surgical period.
Performance Comparison of Wearable Sensors
Recent studies reveal how wearable sensors differ in their ability to meet the clinical demands of fever detection and temperature tracking. Here’s a comparison of key devices:
| Device/Technology | Reference Standard | Mean Bias / Accuracy | Key Performance Finding |
|---|---|---|---|
| iThermonitor (Axillary) | Esophageal Probe | 0.16°C bias; 93.96% within ±0.5°C | 100% sensitivity for detecting hypothermia below 95.9°F |
| SteadyTemp (Patch) | Infrared (Temporal) | N/A | Detected fever in 93.9% of febrile patients compared to 36.4% with infrared |
| iThermonitor WT705 | Mercury Thermometer | 0.03°C ± 0.35°C bias | Detected fever 4.35 hours earlier on average |
It’s worth noting that patient characteristics, such as a low Body Mass Index (BMI below 18.5 kg/m²), can impact sensor accuracy. For example, axillary sensors may show reduced reliability in individuals with lower BMI due to decreased thermal insulation and less effective tissue-probe coupling.
Benefits and Limitations of Wearable Temperature Monitors
Benefits of Wearable Devices
Wearable temperature monitors offer continuous, minute-by-minute data, which helps catch complications like fever spikes much earlier than traditional methods that check every 4–8 hours. In fact, these devices can identify infectious issues up to 14 hours earlier than standard nursing charts.
Their non-invasive design makes them more comfortable for patients, allowing greater mobility during recovery compared to invasive probes. This freedom can be especially important for post-surgical patients who need to move around for better recovery.
When integrated into post-surgical care, wearable devices have shown to improve outcomes. Studies highlight benefits like shorter hospital stays, fewer ICU readmissions, and quicker administration of antibiotics when required. Real-time alerts from these devices also help prevent delays in treatment, while automated wireless data transmission reduces the need for manual data entry, cutting down on errors and staff workload.
However, despite these advantages, wearable monitors have their limitations.
Limitations and Drawbacks
For accurate readings, these devices need consistent contact with the skin. Something as simple as opening the arm can cause temperature readings to drop by 3°F in just one minute. Additionally, when the device is re-applied or reconnected, it takes 5 to 20 minutes to stabilize before providing reliable data.
Patient factors also play a role in performance. For instance, underweight patients (BMI below 18.5) often experience less accurate readings due to poor contact between the sensor and tissue, as well as reduced thermal insulation. Advancements are still needed to improve accuracy for these individuals and those with naturally lower baseline temperatures.
Another challenge is alert fatigue. In one study, the median time to acknowledge an alert was 111 minutes, with some responses taking over 2,000 minutes. Frequent false alerts can cause staff to become disengaged. On top of that, adhesive patches used in these devices can cause temporary skin redness in 45% of surgical patients, and disconnections have led to incomplete temperature data, with some devices only capturing 72.8% of the required data.
Comparison Table of Wearable Technologies
| Technology Type | Primary Advantage | Main Limitation |
|---|---|---|
| Flexible Patches (iThermonitor) | 93.96% accuracy within ±0.9°F and effective fever detection | Higher bias for underweight patients; 45% skin redness incidence |
| Continuous Telemetry (SteadyTemp) | Detected fever in 93.9% of cases compared to 36.4% with infrared thermometry | High risk of accidental removal and detachment |
AI-Powered Wearable Devices for Post-Surgical Recovery
How AI Improves Wearable Health Technology
AI is transforming wearable technology for post-surgical care, especially in monitoring body temperature. By using machine learning algorithms and random forest regression, non-invasive sensors – worn on the wrist or under the arm – can estimate internal core body temperature more accurately. These systems adjust for factors like ambient temperature, body position, physical activity, and the effects of anesthetics, ensuring reliable readings despite external interferences. Advanced filtering techniques, such as combining Moving Average Filters with Kalman filters, further refine data by correcting motion artifacts and systemic errors in real time.
In one study involving 526 surgical patients, AI-powered devices identified 117 febrile events, compared to 91 detected through manual checks, and flagged fever onset up to 4.35 hours earlier. To avoid overwhelming medical staff, these systems incorporate persistence logic, requiring multiple abnormal readings before triggering alerts, and include silencing periods to ensure notifications remain actionable. When wearable data was integrated into clinical AI models, it boosted the precision-recall curve for detecting complications by 109%. Additionally, multimodal AI systems now combine wearable data with electronic health records to predict issues like intra-abdominal infections up to 9 hours before they are clinically recognized, achieving a median AUROC of 0.90.
These advancements highlight the potential of devices like the aiRing to redefine post-surgical monitoring.
AIH LLC‘s aiRing for Post-Surgery Temperature Monitoring
AIH LLC’s aiRing is a prime example of how AI-driven technology is advancing recovery care. This smart ring continuously tracks and analyzes vital signs, including temperature, using autonomous AI algorithms. Its ultra-low-power Bluetooth ensures seamless integration with multiple devices, including the AIH Health App and Remote Therapeutic Monitoring platforms. The ring is designed for everyday use – it’s waterproof and features intuitive touch controls, making it user-friendly for patients during recovery.
The aiRing also supports remote monitoring services, allowing healthcare professionals to track therapy adherence, monitor musculoskeletal or respiratory conditions, and assess recovery progress from a distance. This capability is particularly important as more surgical patients are discharged early, requiring effective home monitoring. Studies have shown that smart rings, due to their placement near arteries and capillaries, achieve superior signal accuracy for vital signs like SpO₂ and blood pressure, with real-world signal acquisition rates exceeding 90%.
Future Development of AI-Integrated Wearables
The next wave of wearable technology aims to integrate continuous physiological data, lab results, and medical history to provide real-time clinical insights. Current advancements in wearable accuracy and early detection are laying the groundwork for predictive care systems that can anticipate complications before they escalate.
"Future systems are expected to evolve into AI-driven platforms that integrate physiological signals, laboratory results, and medical history to provide real-time clinical insights." – Nature Scientific Reports
Researchers are working on AI models to predict specific complications, such as deep surgical site infections and pancreatic fistulas, up to 9–12 hours before they are clinically apparent. For example, the CASSANDRA Study, involving 1,285 surgical patients from 2022 to 2025, demonstrated the potential of such systems. The study’s CASHEWS+ AI model analyzed 13.8 billion PPG data points alongside electronic medical records to predict intra-abdominal infections with an AUROC of 0.90, providing a 9-hour warning. These wearables could form the backbone of "smart wards", where real-time risk stratification reduces the workload on clinical staff. As Robin P. van de Water and colleagues at the Hasso Plattner Institute stated:
"Our results reveal continuous monitoring, using minimally intrusive vital signs, as a key component of an intelligent, data-driven smart ward."
Looking ahead, advancements like nanotechnology may enable wearables to monitor biochemical markers continuously, paving the way for personalized, preventive care. Future devices could even provide real-time insights into a patient’s pain levels by analyzing heart rate variability and activity patterns. Early machine learning models have already achieved 70% accuracy in predicting poor pain relief after orthopedic surgeries. The shift toward machine learning-based alert systems marks a significant step in post-surgical care, moving from reactive to predictive approaches while reducing alarm fatigue and improving outcomes.
Conclusion
Summary of Wearable Temperature Monitoring Benefits
Wearable temperature monitors are reshaping post-surgical care by offering more accurate and timely fever detection compared to traditional methods. For instance, continuous monitoring identifies fever in 93.9% of cases, while infrared thermometers detect it in only 36.4%. Even more impressively, these devices can alert caregivers to febrile events up to 4.35 hours earlier than conventional approaches. They also provide a safer alternative to invasive techniques. At Beijing Tongren Hospital, esophageal probes caused mucosal injuries in 73.8% of cases, whereas wearable devices only resulted in minor skin redness. Beyond safety and accuracy, these monitors enhance patient comfort and mobility. A great example is the MT100D, which received an impressive 4.69/5 satisfaction rating from patients. When paired with AI, these devices take monitoring to the next level, boosting both precision and predictive capabilities.
The Impact of AI-Driven Devices
AI is turning wearable monitors into powerful tools for predictive healthcare, especially in post-surgical recovery. Take the CASSANDRA study conducted at Charité – Universitätsmedizin Berlin, for example. Over three years, researchers monitored 1,136 surgical patients, analyzing 13.8 billion PPG data points alongside temperature readings. This enabled the prediction of complications like deep surgical site infections and bile leaks 9 hours before clinical recognition, achieving an AUROC of 0.89. Devices like AIH LLC’s aiRing highlight how AI-driven wearables are revolutionizing care. Featuring autonomous algorithms and cutting-edge sensors, aiRing provides continuous, real-time monitoring that integrates seamlessly with remote health platforms. These advancements are paving the way for earlier hospital discharges, as patients can be reliably monitored at home.
Future Applications of Wearables in Healthcare
The future of wearable technology in healthcare looks even more promising as AI continues to refine its capabilities. Researchers are already working on systems that can predict complications like pancreatic fistulas or sepsis hours before symptoms appear. These innovations could become the foundation of "smart wards", where continuous digital monitoring helps nursing staff focus on high-risk patients without being overwhelmed by false alarms. Beyond hospital settings, wearables could be used to monitor cancer patients undergoing chemotherapy for early signs of febrile neutropenia, track pediatric patients, or provide long-term care after discharge.
"Our results reveal continuous monitoring, using minimally intrusive vital signs, as a key component of an intelligent, data-driven smart ward."
This evolution from reactive care to predictive care highlights the immense potential of wearables in transforming post-surgical recovery and beyond.
FAQs
Are wearable temperature monitors accurate enough for post-surgery care at home?
Wearable temperature monitors are reliable for post-surgery care at home. Research shows they effectively track temperature continuously and detect early signs of fever. This makes them a useful tool for monitoring recovery, offering consistent readings that help patients and healthcare providers stay informed during the healing process.
What can cause false temperature alerts with wearable patches or rings?
False temperature alerts in wearable devices can happen for several reasons. These include improper sensor placement, movement-related interference, external conditions like extreme heat or cold, or even calibration problems. To reduce the chances of these errors, it’s important to use the device correctly and keep it well-maintained.
How does AI improve fever detection compared with continuous temperature tracking alone?
AI improves the detection of fevers by analyzing continuous temperature data collected from wearable devices. This method enables earlier and more reliable identification of fever compared to traditional intermittent measurements, which can overlook critical temperature changes. With this technology, healthcare providers can track fever onset more effectively, offering more precise and timely insights – especially valuable for monitoring recovery after surgery.